Vitamin D Could Cut Dementia Risk By 40%
FoundMyFitness | May 19, 2025
Vitamin D is far more than just a vitamin—it’s a potent steroid hormone regulating nearly 5% of our genome. Yet, remarkably, up to 70% of Americans aren’t getting enough, placing them at increased risk for dementia and Alzheimer’s disease. In this video, I explore compelling new evidence from a study involving over 12,000 participants, demonstrating that vitamin D supplementation can reduce dementia risk by an impressive 40%, protecting even adults with genetic Alzheimer’s risk (ApoE4 carriers).
EPISODE LINKS
Show notes & transcript: https://www.foundmyfitness.com/episod…
PODCAST INFO
Spotify: https://open.spotify.com/episode/50aP…
Apple Podcasts: https://podcasts.apple.com/us/podcast…
SUPPORT MY MISSION
Get access to more than 65 Ask Me Anything episodes with me when you become a FoundMyFitness Premium Member: https://www.foundmyfitness.com/crowds…
Read the FoundMyFitness Vitamin D topic page for a deeper dive into the science: https://www.foundmyfitness.com/topics… #vitamind
May 21, 2025 Posted by aletho | Science and Pseudo-Science, Timeless or most popular, Video | Vitamin D | Leave a comment
Thinking of taking a flu shot? Read this first… It’s not just that they’re ineffective, they also cause harm.
Learn about safe alternatives such as Vitamin D, quercetin and zinc
World Council for Health | October 15, 2024
If you’re of a certain age or demographic and in the northern hemisphere, chances are you’re being invited or encouraged to get a flu vaccine. The claim is that flu vaccines protect you and others from coming down with flu – and that if you do get it, the symptoms will be mild. So, is this true?
Many scientists see the flu shot as an unnecessary measure. For one thing, there’s a big question over whether the flu vaccine even works, particularly for older people, for whom it is recommended. Studies show that the vaccines often do not match the circulating viruses and no significant effects on serious complications or hospitalizations have been demonstrated.
You’d think that vaccinating people against flu would lead to a reduction in deaths from flu. But figures show that this isn’t the case. In fact, even though the number of flu shots given has increased more than eightfold, the number of flu-associated deaths has remained more or less unchanged.
There’s a logical explanation, and it goes like this:
Antibodies are not enough
Flu vaccines, like any other vaccine, primarily rely on the so-called Th2 antibody response. This generates antibodies to help the body fight off the influenza virus once it enters the bloodstream. What vaccines don’t do is impact the first line of defence in the nasal mucosa. This part of the innate immune system does not use antibodies, and it is here where respiratory viruses replicate.
This is why vaccines for respiratory viruses will never prevent infection or the transmission of the disease.
The immune response to vaccinations also decreases with age, which further reduces the already weak effect of vaccination in older people. Studies bear this out. In particular, a 2012 article in the British Medical Journal quoted an independent study that looked at data from 1967 to 2012 and concluded there isn’t strong evidence showing that the flu vaccine consistently protects people. While it does offer some protection for young, healthy adults who usually don’t face serious flu complications, the researchers noted that there is not enough evidence to support its effectiveness for older adults (65 and older), who account for more than 90% of flu-related deaths.
Recent research into the efficacy of flu shots also reveals their limitations
- In 2020, Anderson et al. showed that influenza vaccination of 60 to 70 year olds in England and Wales had no discernible positive impact on hospitalization or deaths:
- Another study in Japan reported on 83,146 individuals aged 65 years and followed them up over six years. In 2023, the incidence of hospitalization for influenza did not differ significantly by vaccination and the claimed protective effectiveness against incidence waned quickly after four or five months.
- Another 2020 study from Anderson and team analysed data covering 170 million episodes of care and 7.6 million deaths. Turning 65 was associated with a statistically and clinically significant increase in rate of seasonal influenza vaccination. However, no evidence indicated that vaccination reduced hospitalizations or mortality among elderly persons. The study points out that estimates were precise enough to rule out results from many previous studies.
This is not just a concern for the elderly but for all those with weakened immune systems, including those undergoing immunosuppressive treatments, or individuals with chronic health conditions. In such cases, the Th2 response may not produce enough protective antibodies to effectively combat the virus, leading to a higher risk of severe illness.
Here’s another reason to exercise caution of the flu vaccine:
Flu vaccines actually SPREAD the virus
Controlled studies published in the Proceedings of the National Academy of Sciences (PNAS) find that people who receive flu shots emit 630% more flu virus particles into the air compared to non-vaccinated people. In other words, flu vaccines spread the flu!
Physicians for Informed Consent has produced this concise summary of facts that you, your loved ones and your doctor should consider before a potential injection.
All this leads to an important next question:
If the flu shot isn’t a good idea, what is?
The flu shots’ limitations make the prevention and treatment of flu with nutritional supplements like Vitamin D, Quercetin, and Zinc more appealing and safe. These supplements not only enhance the immune response but also offer additional antiviral and anti-inflammatory benefits:
Vitamin D protects the lungs and airways – and much more besides
Studies have shown that Vitamin D supplementation can significantly reduce the risk of influenza infections by enhancing the body’s immune response. It works by modulating the expression of inflammatory cytokines and increasing macrophage function, which are essential for fighting off infections.
Moreover, Vitamin D has been found to protect the lungs and airways through the antimicrobial peptide cathelicidin, which has both antibacterial and antiviral properties. Vitamin D supplementation shows promise in reducing the risk and severity of respiratory infections, including influenza. The evidence suggests that consistent Vitamin D intake can lower the incidence of acute respiratory infections, shorten the duration of symptoms, and enhance immune response, particularly in the elderly. These benefits can translate into reduced hospitalizations and deaths due to flu, making Vitamin D a valuable component in flu prevention and management strategies.
Quercetin: a powerful antiviral and zinc’s vital wingman
Quercetin is a flavonoid found in many fruits and vegetables, known for its antiviral, anti-inflammatory, and antioxidant properties. It has been shown to inhibit the entry and replication of viruses in lung cells, making it a potent candidate for managing respiratory infections like the flu. Quercetin also acts as a zinc ionophore, facilitating the transport of zinc into cells, which enhances its antiviral effects. Studies suggest that the co-administration of Quercetin and Vitamin C can exert a synergistic antiviral action, further boosting immune response and reducing viral replication
Zinc: helps prevent and reduce infection severity and duration
Zinc is an essential mineral that supports various cellular functions of both the innate and adaptive immune systems. It interferes with the process that certain cold viruses use to multiply, thereby reducing the severity and duration of infections. Zinc is particularly important for the recruitment and activity of neutrophil granulocytes, natural killer cells, and T cells, all of which play critical roles in the immune response. Supplementation with zinc has been supported by evidence showing its effectiveness in preventing viral infections and reducing their severity.
In summary…
The questionable efficiency and safety of the flu vaccine raises important concerns that cannot be overlooked. Alternative approaches such as supplementing vitamin D, quercetin and zinc, are one way to enhance immunity without the risks associated with traditional vaccinations.
Moreover, the potential for the production of IgG4 antibodies as a response to the vaccine illustrates a complex interaction between immunization and immune system dynamics, where the very act of repeated vaccination may inadvertently lead to a weakened response against certain influenza strains. This effect can also result in the weakening of the immune system in general to fight infections and cancer. This highlights the need for continued research and dialogue about the benefits and risks of flu vaccination versus alternative preventive strategies.
As we navigate through flu seasons, it is crucial to remain informed and consider individualized approaches to immune health. Ultimately, a well-rounded strategy that includes lifestyle choices, nutritional support, and an understanding of the science behind flu immunization could empower individuals to make informed decisions that best suit their health needs. The World Council for Health stands for a better way.
References:
1. Berndt, Christina: ‘Experten mit den falschen Freunden’, http://www.sueddeutsche.de/wissen/staendige-impfkommission-experten-mit-den-falschen-freunden-1.271784. 49 Arbeitsgemeinschaft Influenza: ‘Was ist die AGI?’
2. http://influenza.rki.de/Arbeitsgemeinschaft.aspx. 50 Robert-Koch-Institut: Epidemiologisches Bulletin, 14.3.2011
3. http://www.gpk.de/downloadp/STIKO_2011_Bulletin10_110314_Schaetzung_der_Influenza_bedingten_Todesfaelle.pdf. 51 World Health Organization: »List of Members of, and Advisor to, the International Health Regulations (2005) Emergency
4. Committee concerning Influenza Pandemic (H1N1), 2009, http://www.who.int/ihr/emerg_comm_members_2009/en/index.html. 52 Jefferson, T.;
5. Di Pietrantonj, C.; Rivetti, A.; Bawazeer, G.A.; Al-Ansary, L.A.; Ferroni, E.: ‘Vaccines for preventing influenza in healthy adults’, in: Cochrane Database of Systematic Reviews, 2010, 7., Art. No.: CD001269, DOI: 10.1002/14651858.CD001269.pub4.
6. Wittig, Frank. Die weiße Mafia: Wie Ärzte und die Pharmaindustrie unsere Gesundheit aufs Spiel setzen, 2012Yan J, Grantham M, Pantelic J, Bueno de Mesquita PJ, Albert B, Liu F, Ehrman S, Milton DK; EMIT Consortium. Infectious virus in exhaled breath of symptomatic seasonal influenza cases from a college community. Proc Natl Acad Sci U S A. 2018 Jan 30;115(5):1081-1086. doi: 10.1073/pnas.1716561115. Epub 2018 Jan 18. PMID: 29348203; PMCID: PMC5798362.
October 18, 2024 Posted by aletho | Science and Pseudo-Science, Timeless or most popular | Quercetin, Vitamin D, Zinc | Leave a comment
Vitamin D and diabetes
Dr. John Campbell • February 7, 2023
Vitamin D and Risk for Type 2 Diabetes in People With Prediabetes, (7th Feb 2023) https://www.acpjournals.org/doi/10.73… HTTPS://WWW.ACPJOURNALS.ORG/DOI/10.73…
Vitamin D has many functions in the body, including a role in insulin secretion and glucose metabolism.
Observational studies, association between low level of vitamin D in the blood, and high risk for developing diabetes.
So, does giving vitamin D to people who were at high risk for diabetes reduce the risk?
Authors searched 3 databases, through 9 December 2022
Compare the use of vitamin D versus placebo for diabetes prevention, in adults with prediabetes.
Meta analysis and reanalysis of pooled data Trials were at low risk for bias
Results Over 3 years of follow-up Vitamin D group New-onset diabetes occurred in 22.7%
Placebo group New-onset diabetes occurred in 25%
Translates to being 15% reduction
Number needed to treat to prevent one case of diabetes 30 adults with prediabetes to prevent 1 person from developing diabetes.
Risk reduction by blood levels
At least 125 nmol/L (≥50 ng/mL) group 50 to 74 nmol/L (20 to 29 ng/mL) group
Cholecalciferol reduced risk for diabetes by 76% (hazard ratio, 0.24)
3-year absolute risk reduction of 18.1% Vitamin D increased the likelihood of regression to normal glucose regulation by 30%
Doses used 20,000 units of cholecalciferol (vitamin D3) weekly
4000 units of cholecalciferol daily 0.75 micrograms of eldecalcitol, (synthetic analogue of vitamin D)
Adverse events
Rare, study could not draw any definite conclusions about safety kidney stones hypercalcemia hypercalciuria
Implications In adults with prediabetes, vitamin D was effective in lowering the risk for developing diabetes.
By the Numbers:
Diabetes in America https://www.cdc.gov/diabetes/health-e…
Total Diabetes From 2001 to 2020, diabetes prevalence significantly increased among over 18s 37.3 million people have diabetes (11.3% of the US population).
28.7 million people have been diagnosed with diabetes.
8.5 million people who have diabetes have not been diagnosed (do not know they have it)
Total Prediabetes 96 million US adults have prediabetes.
Cost of Diabetes (2017) $327 billion, $237 billion direct medical costs $90 billion in lost productivity
Excess medical costs, $9,601 per person https://www.diabetes.org.uk/professio…
UK prevalence 4.8 million (7%)
3.9 million diagnosed
1 million undiagnosed
5.3 million by 2025 People with type 2 diabetes
50% more likely to die prematurely
Two-and-a-half times more likely to develop heart failure
Twice more likely to have a heart attack
February 20, 2023 Posted by aletho | Economics, Science and Pseudo-Science, Timeless or most popular, Video | carbohydrates, exercise, Obesity, processed foods, sugars, UK, United States, Vitamin D | Leave a comment
The Latest Vitamin D Study is Kinda Stunning! *Viral Revelations*
The Fat Emperor – Ivor Cummins | February 7th, 2022
Not one to miss – the latest Israeli Vitamin D status vs Covid Severity study is not only stunning, but agrees with the similar studies I featured in April 2020!
Please subscribe and share! Odysee Channel: https://odysee.com/@IvorCummins:f
NOTE: My extensive research and interviewing / video/sound editing and much more does require support – please consider helping if you can with monthly donation to support me directly, or one-off payment:https://www.paypal.com/donate?hosted_button_id=69ZSTYXBMCN3W
- alternatively join up with my Patreon:https://www.patreon.com/IvorCummins
…
https://www.youtube.com/watch?v=HLvDkYr3GaY
February 9, 2022 Posted by aletho | Science and Pseudo-Science, Timeless or most popular | Covid-19, Vitamin D | Leave a comment
This Nutrient Deficiency Is Associated With Depression
By Dr. Joseph Mercola | December 27, 2021
Research published in December 20211 using data from the Irish Longitudinal Study on Aging (TILDA) discovered those with a vitamin B12 deficiency had a greater risk of symptoms of depression. According to the Anxiety and Depression Association of America,2 264 million people worldwide live with symptoms of depression. In 2017, roughly 17.3 million adults in the U.S. had experienced at least one major depressive episode.
This number rose in 2019 to 19.4 million adults who had experienced at least one major depressive episode.3 It is not uncommon for someone who has depression to also suffer from symptoms of anxiety.4 According to the CDC,5 data from the National Health and Nutrition Examination Survey show women are roughly twice as likely to experience depression as men, which was a pattern that was observed in each age group surveyed.
Symptoms of depression can include feeling sad or empty, hopeless, irritable, worthless and restless. You may have difficulty sleeping, experience appetite or weight changes or have thoughts of death or suicide. Not everyone experiences every symptom. For some individuals, their symptoms make it difficult to function.6
The December 2021 study linked deficiencies in vitamin B12 with the incidence of symptoms of depression in the elderly. Vitamin B12 is a water-soluble vitamin found in some foods.7 It’s also available as a prescription medication and dietary supplement. Your body uses vitamin B12 for the function and myelination of the central nervous system, to form healthy red blood cells and in DNA synthesis.
Food sources include those of animal origin, such as pasture-raised poultry, dairy products, eggs and meat. Absorption of vitamin B12 is dependent on intrinsic factor, which is a transport and delivery binding protein produced in the stomach.8 The bioavailability from food decreases when the amount of vitamin B12 exceeds the capacity of intrinsic factor.
Vitamin B12 is released from food by the activity of hydrochloric acid and gastric protease in the stomach and saliva in the mouth.9 In 1999 it was estimated10 that vitamin B12 deficiency affects up to 15% of people over age 60. In this study, however, classic symptoms of deficiency were often lacking in this population.
The low vitamin B status is attributed to the high prevalence of atrophic gastritis which results in low-acid pepsin secretion and reduces the release of vitamin B12 from food. The 2021 study finds these low levels of vitamin B12 may increase the risk of depression in older adults.11
Vitamin B12 Deficiency Associated With Depression
The study published in the British Journal of Nutrition12 sought to evaluate the relationship between vitamin B12, folate and the incidence of depression in older individuals living in the community. There were 3,849 individuals over age 50 included.
The results showed a link between vitamin B12 deficiency, but not with a folate deficiency.13 The researchers found that even after controlling for factors such as chronic disease, cardiovascular disease, antidepressant use, physical activity and vitamin D status, the results remain significant.14
The older adults who had a B12 deficiency had a 51% increased risk of developing symptoms of depression during the four years of the study. The data also showed that certain factors influenced the vitamin B12 status in older adults. This included geographic location, obesity, smoking, socioeconomic status and gender.
While the link was found between older adults living in the community and a vitamin B12 deficiency, they also found that older individuals in the study had a lower risk of depression. In a press release from Trinity College Dublin, Eamon Laird, from TILDA15 and lead scientist of the study talked about the results in a press release, saying:16
“This study is highly relevant given the high prevalence of incident depression in older adults living in Ireland, and especially following evidence to show that one in eight older adults report high levels of low B12 deficiency rates.
There is a growing momentum to introduce a mandatory food fortification policy of B-vitamins in Europe and the UK, especially since mandatory food fortification with folic acid in the US has showed positive results, with folate deficiency or low status rates of just 1.2% in those aged 60 years and older.”
Vitamin D Deficiency Plays a Role in Mental Health
This recent study highlights the importance of adequate nutrition to protect your optimal health. In addition to vitamin B12, other nutrients have a significant effect on mental health. Vitamin D is one of those nutrients. Vitamin D, also known as calciferol,17 is a fat-soluble vitamin, which your body can absorb from a few foods and produces endogenously when exposed to sunlight.
People can become deficient when they consume less than the recommended level, have limited exposure to sunlight, their absorption from the digestive tract is inadequate, or the kidneys do not convert the vitamin to its active form. Scientists believe that vitamin D deficiency is a vastly overlooked global health problem at epidemic proportions.18
How vitamin D deficiency is defined also varies. For the most part, researchers interpret vitamin D deficiency as serum levels of 25(OH)D at 20 nanograms per milliliter (ng/mL) or less.19 However, optimal serum levels of vitamin D are between 40 ng/mL and 60 ng/mL.20
Early research in 200021 demonstrated there were significantly deficient levels of vitamin D3 in patients who suffered from depression and alcohol addiction. By 2007, researchers had recognized the importance of low levels of vitamin D on mood.22
Further research23 found individuals with fibromyalgia also had a higher risk of low serum levels of vitamin D and it appeared that supplementing with high doses of vitamin D in individuals who were depressed and overweight could ameliorate the symptoms.24 Over the years, researchers continue to ask the question if vitamin D is a causal association with depression or another symptom of the condition.25
Other scientists postulated whether an effective therapy for depression would be the detection and treatment of vitamin D deficiency.26 By 2014,27 one study found hypovitaminosis D was associated with the severity of depression that people experienced. Their results suggested there was an inverse associated dose-response, which implied that low levels of vitamin D may be an underlying biological vulnerability.
In 2018,28 the British Journal of Psychiatry published a systematic review and meta-analysis that demonstrated low levels of vitamin D are associated with depression. The important factor to remember is that it’s highly unlikely supplementation in people whose serum levels are optimal will have any effect on mood disorders. Instead, the effect is more likely to be found in those whose serum levels are low.
Relevance of Omega-3 Fatty Acids for Depression
Omega-3 fats are essential polyunsaturated fatty acids (PUFAs), which your body needs for a variety of functions. These include digestion, blood clotting, brain health and muscle activity. In early 2021, omega-3 fats made the news when data29 revealed individuals with an omega-3 index measuring 5.7% or greater had significantly better outcomes from COVID-19.
An omega-3 index measures the amount on the red blood cell membranes.30 Those with a measurement less than 4% have a higher risk of heart disease. Individuals with an omega index between 4% and 8% have an intermediate risk and those whose level is greater than 8% are at low risk of heart disease.
One 2016 published analysis of the data31 revealed there were areas of the world with omega-3 index measurements greater than 8%. These included Scandinavia, Sea of Japan and indigenous populations who did not eat westernized foods. Areas of the world with levels below 4% included Central and South America, Europe, North America, the Middle East, Southeast Asia and Africa.
While your level of omega-3 is important, equally as important is the ratio between omega-6 and omega-3. I have found it extremely difficult to correct an imbalance by simply taking more omega-3 fats. In fact, just as an excessive amount of omega-6 is dangerous, an excessive amount of omega-3 can also contribute to ill-health.
The imbalance between omega 6 and omega 3 that occurred in the last 150 years is thought to be behind many of the inflammatory-related diseases common in society, including depressive disorders.32 Increasing evidence suggests that a deficiency in omega-3 fats contribute to mood disorders, including depression.33,34,35
Increased Risk in Elderly of Deficiencies and Depression
Vitamin D,36 B1237 and omega-3 fats are common deficiencies found in the general population and older adults. The reason older adults may have nutrient deficiencies is likely related to poor absorption, poor diet and lack of exposure to sunlight.
A lack of optimal levels of nutrients is a significant contributor to the development of inflammation and disease, and one of the health conditions associated with inflammation is depression.38 Depression affects the quality of life and productivity in the elderly, at a time when they are often more isolated from others.
To date, many older adults are treated for depression using psychotherapy and/or medications. However, since there is a significant link between nutrition and mood, it only makes sense to first address the potential nutrient deficiencies before adding medications that come with a long list of side effects.
One of the more common classes of antidepressants, selective serotonin reuptake inhibitors (SSRIs),39 may trigger nausea, dizziness, insomnia, anxiety, diarrhea and tremors,40 all of which can be dangerous for older adults. These side effects can negatively impact intake or increase the risk of a fall.
As has been demonstrated during the COVID-19 pandemic, maintaining optimal health and nutrition helps to reduce your risk of contracting a viral illness. The featured study also demonstrates that nutrient intake is crucial to your mental health. It is much easier to address bodily needs before they trigger illness and disease. Although it may take a little time and energy, it is vital for your quality of life to take control of your health.
Sources and References
- 1, 12 British Journal of Nutrition, 2021; doi:10.1017/S0007114521004748
- 2 Anxiety and Depression Association of America, Depression
- 3 National Institute of Mental Health, Major Depression
- 4 Anxiety and Depression Association of America, Facts and Statistics
- 5 Centers for Disease Control and Prevention, February 2018
- 6 National Institute of Mental Health, Depression, section 2
- 7, 8, 9 National Institutes of Health, Vitamin B12
- 10 Annual Review of Nutrition, 1999;19:357
- 11, 13 Technology Networks, December 15, 2021
- 14, 16 Trinity College Dublin, December 14, 2021
- 15 Trinity College Dublin, The Irish Longitudinal Study on Aging
- 17 National Institutes of Health, vitamin D
- 18 International Journal of Health Sciences, 2010; 4(1)
- 19 European Journal of Clinical Nutrition, 2020; 74
- 20 Grassroots Health, Are You Vitamin D Deficient?
- 21 Journal of Neural Transmission, 2000; 107
- 22 Medical Hypothesis, 2007; 69(6)
- 23 Clinical Rheumatology, 2007; 26
- 24 Journal of Internal Medicine, 2008; doi.org/10.1111/j.1365-2796.2008.02008.x
- 25 Nutrition Reviews, 2009;67(8)
- 26 Issues in Mental Health Nursing, 2010;31(6)
- 27 Molecular Psychiatry, 2014; 19
- 28 British Journal of Psychiatry, 2018; 202(2)
- 29 Prostaglandins, Leukotrienes and Essential Fatty Acids, 2021; doi.org/10.1016/j.plefa.2021.102250 Highlights
- 30 OmegaQuant, July 9, 2018, Risk Zones
- 31 Progress in Lipid Research, 2016; 63
- 32 Oxidative Medicine and Cellular Longevity, 2014; (313570)
- 33 Critical Reviews in Food Science and Nutrition, 2017; 57:1
- 34 Frontiers in physiology, 2018; doi.org/10.3389/fphys.2018.01047
- 35 Translational Psychiatry, 2019;9(190)
- 36 Avicenna Journal of Medicine, 2018;8(4)
- 37 Hong Kong Medical Journal 2015;21(2)
- 38 Frontiers in Immunology, 2019;10(1696)
- 39 NIH MedlinePlus, 2020
- 40 Cleveland Clinic, Depression Medications
December 27, 2021 Posted by aletho | Science and Pseudo-Science, Timeless or most popular | Vitamin B12, Vitamin D | Leave a comment
Vitamin D: Government Should Have Promoted to Combat Pandemic
Medical evidence strongly justifies a proactive approach for using vitamin D
By Joel S Hirschhorn | December 4, 2021
There seems to be an endless refusal by the public health establishment to fight the pandemic with the best science-based tools. Instead, they keep pushing vaccines.
Great German research provides unequivocal medical evidence that the government should be strongly advocating two actions: 1. Take vitamin D supplements and 2. Have your blood tested for vitamin D.
The title for this October 2021 journal article says it all: “COVID-19 Mortality Risk Correlates Inversely with Vitamin D3 Status, and a Mortality Rate Close to Zero Could Theoretically Be Achieved at 50 ng/mL 25(OH)D3: Results of a Systematic Review and Meta-Analysis.” [25(OH)D3 refers to metabolite of the vitamin in blood]
In other words, there is clear evidence that the lower your vitamin D level the greater your risk of dying from COVID infection. Moreover, the data clearly show that you need a blood level of at least 50 ng/mL.
Odds are, however, that very, very few people have been tested for their vitamin D level. This is a situation where waiting for testing is not the prudent approach. Vitamin D pills are pretty cheap and it is perfectly safe to take a healthy daily dose to maintain a good immune system. I take 4,000 IUs twice daily.
Here are a number of highlights from this research and other sources; the discussion is aimed at informing people with information not provided by Big Media, Big Government and Big Pharma.
Vitamin D is an accurate predictor of COVID infection. Its deficiency is just as significant, and perhaps more so, than more commonly discussed underlying medical conditions, including obesity.
To be clear, there is a level of vitamin D for an effective strategy at the personal and population level to prevent or mitigate new surges and outbreaks of COVID that are related to reduced vaccine effectiveness and new variants.
In the German study, fifteen other studies were cited that showed low vitamin D levels were related to cases of severe COVID infection, and seven studies that found positive results from treating ill patients with the vitamin.
The German study noted: “The finding that most SARS-CoV-2 patients admitted to hospitals have vitamin D3 blood levels that are too low is unquestioned even by opponents of vitamin D supplementation.” The German study “followed 1,601 hospitalized patients, 784 who had their vitamin D levels measured within a day after admission and 817 whose vitamin D levels were known before infection. And the researchers also analyzed the long-term average vitamin D3 levels documented for 19 countries. The observed median vitamin D value over all collected study cohorts was 23.2 ng/mL, which is clearly too low to work effectively against COVID.”
Why does this vitamin work so well? The German study explained: A main cause of a severe reaction from COVID results from a “cytokine storm.” This refers to the body’s immune system releasing too many toxic cytokines as part of the inflammatory response to the virus. Vitamin D is a main regulator of those cells. A low level of the vitamin means a greater risk for a cytokine storm. This is especially pertinent for lung problems from COVID.
Other studies
On a par with the German study was an important US medical article from May 2021: Vitamin D and Its Potential Benefit for the COVID-19 Pandemic. It noted: “Experimental studies have shown that vitamin D exerts several actions that are thought to be protective against coronavirus disease (COVID-19) infectivity and severity. … There are a growing number of data connecting COVID-19 infectivity and severity with vitamin D status, suggesting a potential benefit of vitamin D supplementation for primary prevention or as an adjunctive treatment of COVID-19. … there is no downside to increasing vitamin D intake and having sensible sunlight exposure to maintain serum 25-hydroxyvitamin D at a level of least 30 ng/mL and preferably 40 to 60 ng/mL to minimize the risk of COVID-19 infection and its severity.” This confirms the German study and its finding of a critical vitamin level of 50 ng/mL.
Daniel Horowitz has made this correct observation about vitamin D supplementation: “An endless stream of academic research demonstrates that not only would such an approach have worked much better than the vaccines, but rather than coming with sundry known and unknown negative side effects.“
There are now 142 studies vouching for the near-perfect correlation between higher vitamin D levels and better outcomes in COVID patients.
From Israel came work that showed 25% of hospitalized COVID patients with vitamin D deficiency died compared to just 3% among those without a deficiency. And those with a deficiency were 14 times more likely to end up with a severe or critical condition.
Also from Israel, data on 1,176 patients with COVID infection admitted to the Galilee Medical Center, 253 had vitamin D levels on record and half were vitamin D-deficient. This was the conclusion: “Among hospitalized COVID-19 patients, pre-infection deficiency of vitamin D was associated with increased disease severity and mortality.”
Several studies have come from the University of Chicago. One found that a vitamin D deficiency (less than 20 ng/ml) may raise the risk of testing positive for COVID-19, actually a 7.2% chance of testing positive for the virus. And that more than 80% of patients diagnosed with COVID-19 were vitamin D deficient. And Black individuals who had levels of 30 to 40 ng/ml had a 2.64 times higher risk of testing positive for COVID-19 than people with levels of 40 ng/ml or greater.
On the good news side is a new study from Turkish researchers. They focused on getting people’s levels over 30 ng/mL with supplements. At that level there was success compared to people without supplementation. This was true even if they had comorbidities. They were able to achieve that blood level within two weeks. Those with no comorbidities and no vitamin D treatment had 1.9-fold increased risk of having hospitalization longer than 8 days compared with cases with both comorbidities and vitamin D treatment.
Another option
Some people may have absorption problems. The solution is to use the active form of D – either calcifediol or calcitriol – to raise their levels more quickly. This bypasses the liver’s metabolic process very effectively. Studies have shown that people hospitalized with low levels but given the active form of D did not progress to the ICU. Places that sell vitamin D often sell the concentrated active form.
I have a supply of cholecalciferol pills that provide 50,000 IUs, compared to ordinary D pills typically with 2,000 IUs. A reasonable use of the high concentration pills is in the event of coming down with a serious COVID infection. This may be a sensible strategy for those who do not know what their level is or have not taken the normal pills for some period. It can take months to raise a very low level to above the critical level the German study found necessary for the best protection.
Deficiency
Aside from dealing with COVID, two pertinent questions are: Is there an optimal level of vitamin D and are Americans deficient in it? For the first, this has been said: “While blood levels of 30 ng/mL or higher are considered normal, the optimal blood level of vitamin D has not yet been established.” From the Cleveland Clinic is this: “Normal vitamin D levels are usually between 20-80 NG/ML. If supplementation is recommended, remember to take it with a meal and on a full stomach to help absorption. Unfortunately, about 42% of the US population is vitamin D deficient with some populations having even higher levels of deficiency.”
A Mayo Clinic study said this: “Vitamin D deficiency is more common than previously thought. The Centers for Disease Control and Prevention has reported that the percentage of adults achieving vitamin D sufficiency as defined by 25(OH)D of at least 30 ng/mL has declined from about 60% in 1988-1994 to approximately 30% in 2001-2004 in whites and from about 10% to approximately 5% in African Americans during this same time. Furthermore, more people have been found to be severely deficient in vitamin D [ <10 ng/mL]. Even when using a conservative definition of vitamin D deficiency, many patients routinely encountered in clinical practice will be deficient in vitamin D.”
Clearly, personal deficiency can only be determined by a blood test that prudent people will request their doctors to order for a lab test.
Conclusions
Seeing vitamin D as crucial to surviving COVID is supported by solid medical research. There is good data to support a desired level of 50 ng/mL. Whether a person has this level requires a blood test for the vitamin, not something that most physicians normally call for when ordering blood tests for other reasons.
As the US approaches 800,000 COVID related deaths it is reasonable to believe that perhaps hundreds of thousands of lives could have been saved if the government had strongly supported vitamin D blood testing and supplementation if needed. But in the absence of such a COVID policy, people have good reasons to use D supplements if they are not routinely exposed to sunlight without using sunscreen products.
Many physicians have issued protocols for preventing and treating COVID that include vitamin D supplements. For example, the esteemed Dr. Zelenko uses the following: 5,000 IU 1 time a day for 7 days for low risk patients, and for high risk patients: 10,000 IU once a day for 7 days or 50,000 IU once a day for 1-2 days.
However, continuing its stupidity, NIH maintains that “There is insufficient evidence to recommend either for or against the use of vitamin D for the prevention or treatment of COVID-19.” This too was said: “Vitamin D deficiency (defined as vitamin D ≤20 ng/mL) is common in the United States, particularly among persons of Hispanic ethnicity and Black race. These groups are also overrepresented among cases of COVID-19 in the United States. Vitamin D deficiency is also more common in older patients and patients with obesity and hypertension; these factors have been associated with worse outcomes in patients with COVID-19.” Sounds smart to fight deficiency for avoiding COVID health impacts.
Sadly, we cannot count on the public health establishment to take a science-based, aggressive policy on using vitamin D supplements as an alternative to COVID vaccines or expensive medicines. Its up to individuals to protect their own lives by being well informed and proactive.
December 4, 2021 Posted by aletho | Science and Pseudo-Science, Timeless or most popular | Covid-19, Vitamin D | Leave a comment
Covid-19: a new look at vitamin D
By Sebastian Rushworth, M.D. | December 3, 2021
I’ve written about vitamin D as a potential treatment for covid-19 a couple of times before. In September of 2020 I wrote about a Spanish randomized trial that showed a massive reduction in ICU admissions in hospitalized patients treated with 25-hydroxyvitamin D (a part-activated form of vitamin D). However, that study had some major weaknesses – it was completely unblinded and it was small. In other words, although the results were promising, they hardly constituted conclusive proof of a benefit.
Then, in January, I wrote about a much larger double-blind Brazilian trial that failed to show any benefit when hospitalized patients were treated with vitamin D. For many in the mainstream medical community, this study constituted conclusive proof that vitamin D is ineffective as a treatment for covid-19. However, participants in the trial weren’t given vitamin D until late in the disease course, and unlike in the previous Spanish study, they were given regular vitamin D, not the part-activated form used in the Spanish study. Since it takes several days for regular vitamin D to become activated and usable by the body, the study was more or less designed to fail from the start – whether intentionally or unintentionally. There was no realistic chance that it was ever going to show a benefit, even if one exists.
So, when I last wrote about vitamin D, in January, it was still unclear whether it had any role in the treatment of covid-19 or not. Well, has anything changed since then?
Let’s start by taking a look at the observational data. Although the randomized trials of vitamin D have been few and far between, there has been a massive amount of observational data produced. In recent months, two meta-analyses of cohort studies have been published that look at the relationship between vitamin D levels and death, one in the journal Nutrients, and another in the Nutrition Journal. For those who are unaware, a meta-analysis is a pooled study, where you take lots of different studies and pool their results together in to one, in order to get more statistically significant results. And a cohort study is a type of observational study in which you take two or more groups that vary in some specific way, such as in their vitamin D levels, and then follow them over time to see if they have different outcomes.
Interestingly, the two meta-analyses reach the exact opposite conclusions, with one claiming that if we can just get everyone up to 50 ng/ml of vitamin D in the blood stream, then we can literally prevent all covid deaths, while the other says that there is no correlation whatsoever between vitamin D levels and covid mortality.
How is this possible?
Well, the first thing to note is that the two meta-analyses vary in terms of which particular studies they include. The Nutrients study performed its data search in March, while the Nutrition Journal study performed its data search in June. This means that the Nutrition Journal meta-analysis had access to a few extra studies, which weren’t available when the first data search was conducted in March.
But that isn’t the whole explanation. The researchers have also used somewhat different search strategies, which means that each includes some studies that the other lacks. In fact, there is amazingly little overlap between the two meta-analyses in terms of which studies are included. Only two of the seven studies in the Nutrients meta-analysis are included in the Nutrition Journal meta-analysis, and only two of the eleven studies in the Nutrition Journal meta-analysis are included in the Nutrients meta-analysis. No wonder they’re able to reach such divergent results!
This really showcases how easy it is to manipulate meta-analyses so that they show what you want them to show, just by choosing the date on which you extract data and by choosing which specific search terms to use. It’s easy to keep modifying search terms slightly until you get a list that includes the studies you want in, and excludes the studies you want out. Which is why we should always be skeptical of meta-analyses, just as we are with other types of studies.
This explains why we saw a similar phenomenon earlier this year, when half the meta-analyses of ivermectin seemed to show massive benefit and the other half seemed to show no benefit whatsoever.
Meta-analyses are often considered to be the pinnacle of evidence based medicine, but considering how easy they are to game, I think that is wrong. I’d rather have a single large, well done study than a meta-analysis that consists of lots of little studies, even if that meta-analysis includes more participants overall. If all scientists were honest, then meta-analyses would be an excellent tool for determining the truth. But since we know that many scientists aren’t honest, their use is far more limited. At the end of the day we all have to do our own due diligence. The only meta-analyses that I trust fully are the ones I do myself, such as one I did earlier this year on ivermectin.
It is interesting to note though, that the Nutrition Journal study, which came to the conclusion that vitamin D had no effect, actually had results that did suggest benefit. All the included studies showed fewer deaths in the group with a higher vitamin D level, although the results were not able to reach statistical significance overall.
So we have one meta-analysis which shows a large benefit, and one which shows a trend towards benefit. Which is encouraging. Of course, these are observational studies, and so can’t really say anything about cause and effect. People with low vitamin D levels probably spend less time outdoors, which means they’re probably less physically active. And they probably consume a different diet from people with high vitamin D levels. Correlation is not causation, and even if a correlation is seen between vitamin D and death from covid in observational studies, that doesn’t mean it’s the vitamin D that’s preventing the deaths.
So, what we need is good data from randomized trials. As mentioned, the data from randomized trials that existed last time I wrote about vitamin D was limited and mixed, with the Spanish study that gave 25-hydroxyvitamin D showing massive benefit, while the Brazilian study that gave regular inactivated vitamin D showed no benefit whatsoever.
Since then, three new randomized trials have been published, one from India, one from Mexico, and one from Saudi Arabia. Unfortunately, all three were small, with the largest of the three only including 87 patients. Additionally, all three gave regular inactivated vitamin D, not the part-activated form that was found to have an effect in the earlier Spanish study. In other words, the new studies don’t add anything on top of the store of knowledge that we already had in January.
So, we’re actually more or less in the same situation that we were in regarding vitamin D back in January. The observational data suggests that there is a benefit to supplementing with regular vitamin D for prophylaxis, which is in line with a systematic review that was published in the British Medical Journal in the pre-covid era, which found that people with low vitamin D levels who supplement daily with vitamin D reduce the frequency of respiratory infections by half. And the limited randomized trial data that exists suggests that the part-activated 25-hydroxyvitamin D formulation can reduce the risk of bad outcomes if given on admission to hospital. But the evidence is still too weak to draw any firm conclusions.
It’s quite shocking that more data isn’t available to answer this question conclusively at this late stage in the pandemic. I do personally think though, based on the evidence that is available, that it makes sense to take a daily vitamin D supplement. 4,000 IU (100 mcg) is a reasonable dose. It’s safe, it’s cheap, it might well help, and it can’t hurt.
December 3, 2021 Posted by aletho | Deception, Science and Pseudo-Science, Timeless or most popular | Covid-19, Vitamin D | Leave a comment
Why Is Info on COVID and Vitamin D Deficiency Suppressed?
By Dr. Joseph Mercola | October 4, 2021
Many years of research have demonstrated the multiple benefits of vitamin D to your health. These benefits include helping to build healthy bones and teeth,1,2 supporting lung3,4 and cardiovascular function,5,6 influencing genetic expression,7,8 supporting brain and nervous system health9,10 and regulating insulin levels.11
During 2020, scientists also discovered that the benefits of vitamin D for upper respiratory infections also include protection against COVID-19.12,13 In 2021, two new studies14,15 confirmed what many researchers had already determined: There is an association between vitamin D deficiency and “the risk of being infected with COVID-19, severity of the disease and risk of dying from it.”16
However, despite a known and safe side effect profile, benefits to patients with COVID-19 and the relative ease of acquiring the low-cost supplement, health “experts” have continued to suppress information that could very well save many lives. To achieve vitamin D toxicity, a person must take more than 40,000 international units (IU) each day and have a serum level above 500 to 600 nanograms per milliliter (ng/ml).17
In addition to this they must also be taking excessive amounts of calcium to experience vitamin D toxicity. In other words, it’s more difficult to overdose on vitamin D than it is to overdose on acetaminophen (Tylenol). Taking more than 3,000 milligrams (mg) of acetaminophen in one day18 can lead to symptoms of an overdose. Signs of toxicity can begin in as little as 30 minutes after ingestion.19
Additionally, it is not difficult to overdose on acetaminophen since it is an ingredient in many over-the-counter cold preparations. Many people who take the drug each week are unaware it is found in combined products.20 The drug is responsible for 500 deaths, 56,000 visits to the emergency room and 2,600 hospitalizations each year.
According to experts, 50% of these injuries are from unintentional overdoses. By contrast, research has found that vitamin D toxicity is rare21 and usually caused by formulation errors, inappropriate prescribing, accidental dispensing or inappropriate administration.22
However, toxicity is not defined consistently across studies. One Irish study found a prevalence of 4.8%, but they considered an elevated result anything above 50 ng/mL (125 nmol/L),23 which is within the normal range of 40 ng/ml to 60 ng/ml.24 Another comparison is that, while studies have shown that the prevalence of vitamin D deficiency25 is 41.6% in the overall population and as high as 82.1% in people with dark skin, there is no known deficiency for acetaminophen.
Vitamin D Deficiency Linked With COVID-19 Severity
One of the newer studies was published in June 2021.26 The researchers sought to determine the role that vitamin D may play in mitigating the impact that SARS-CoV-2 has on morbidity and mortality. They recognized that the production of vitamin D through sensible sun exposure is often limited by geographical location.
Clothing, sunblock and skin pigmentation also limit vitamin D production in the skin. Serum levels of 25-hydroxyvitamin D have been found suboptimal in adults from many countries and are not limited to specific risk groups. The study used an ecological design to find an association and looked at complications and mortality in 46 countries.
They used data from public sources to look for and find evidence of a vitamin D deficiency, which they defined as serum levels less than 20 ng/ml. Although lower than optimal levels for vitamin D, this has been a deficiency level consistently used by researchers.
The researchers gathered data from Worldometer on the number of cases, tests and deaths in a population. They found a statistically significant correlation between deficiency and infection and fatality.
Data analyses were not limited to a specific area of the world or population group but instead included data from 46 countries. The data from this study supported a review of evidence published in Nutrients in 2020 that demonstrated vitamin D levels were associated with:27
- A lower number of cases in the Southern Hemisphere
- An association with deficiency and the development of acute respiratory distress syndrome
- An increase in mortality rates in older adults and patients with chronic diseases that are associated with vitamin D deficiency
- Outbreaks during the winter months when serum levels of vitamin D are lowest
They concluded the data suggest28 “that vitamin D deficiency is associated with an increased risk of COVID-19 infection and mortality across a wide range of countries.”
Second Study Has Similar Results
A second study was published in September 2021 from Trinity College and the University of Edinburgh.29 These researchers also looked at the association between COVID-19 and vitamin D levels. What they found was that the level of ambient ultraviolet B light at a person’s home in the weeks before infection “was strongly protective against severe disease and death.”30
The study was published in the journal Scientific Reports.31 The researchers identified the association from data pulled from 417,342 records stored in the U.K. Biobank. This is a large-scale database that contains in-depth information on genetics and health from a half-million participants.32
From this cohort there were 1,746 cases and 399 deaths registered from March 2020 to June 2020. Unfortunately, on average, vitamin D levels were measured approximately 11 years before the pandemic. Therefore, the researchers looked at ambient UVB light that they found was strongly and inversely associated with hospitalization and death.33
These studies support and confirm earlier research published in 2020 and 2021 that demonstrate a strong association between vitamin D status and infection, hospitalization and death from COVID-19. Early papers published in May 2020,34 offered ample evidence that “vitamin D deficiency to address COVID-19 warrant aggressive pursuit and study.”35
By October 2020,36 research had revealed that people with vitamin D deficiency are at higher risk during the global pandemic and that supplements should be used to maintain circulating 25 hydroxyvitamin D at optimal levels. Retrospective data demonstrated that a deficiency was also associated with an increased risk of COVID1-19 infection.37
In a group of frail elderly nursing home residents with COVID-19 in France,38 researchers found that providing a bolus of vitamin D3 during illness or in the month prior had a significant impact on the severity of the illness and improved survival rates.
Further studies found similar results demonstrating that vitamin D deficiency was associated with increased severity and mortality39 and that supplementation may increase immunity and decrease susceptibility to the infection.40
Information Suppressed Despite Mounting Evidence
Despite mounting evidence that a simple and effective strategy was available to help reduce illness and mortality, health agencies sought to suppress the information. In the early months, many questioned the organized effort to create a situation in which more people were dying.
And yet, as the year wore on, it became more evident that U.S. health officials were intent on ensuring the highest number of people possible would take a genetic therapy experiment to protect themselves against a virus for which treatment protocols and preventive measures had been identified. The aim of some agencies was to put an end to Mercola.com. In the summer of 2020, the Center for Science in the Public Interest (CSPI) launched a social media campaign to that end.41
It’s important to note that this self-proclaimed consumer advocacy group is partnered with Bill Gates’ agrichemical PR group, the Cornell Alliance for Science,42 and is bankrolled by the Rockefeller Foundation, the Rockefeller Family Fund, Public Welfare Foundation, Tides Foundation and Bloomberg Philanthropies.43
The CSPI released a press release July 21, 2020,44 in which they falsely accused me of profiteering from the pandemic by selling “at least 22 vitamins, supplements and other products” to “prevent, treat or cure COVID-19 infection.”
However, in their own Appendix of Illegal Claims, it clearly shows that there are no COVID-19 related claims that exist on any of the products themselves. Rather, the links that CSPI uses go to Mercola articles and interviews — none of which are used to sell anything.45
NOTE: It is wise not to click on CSPI’s shortened links in the “website links” column as they do not currently point to Mercola.com product pages.
Three weeks later, CSPI president Dr. Peter Lurie46 sent an email August 12, 2020, to CSPI’s newsletter subscribers in which he repeated the spurious claim that I “profit from the COVID-19 pandemic” through “anti-vaccine fearmongering” and reporting of science-based nutrition shown to impact your disease risk.
CSPI Takes Public Credit for FDA Action
Interestingly, Lurie is a former FDA associate commissioner.47 It’s disheartening, but not surprising, that the FDA followed up with a warning letter in February 2021,48 for “Unapproved and Misbranded Products Related to Coronavirus Disease 2019.”
Lurie has publicly taken credit for this action,49 and thereby establishes the potential that CSPI is pulling the strings under the new administration through relationships they did not have in July 2020 when they first launched their assault on my free speech.
According to the letter, the FDA lists liposomal vitamin C, liposomal vitamin D3 and quercetin products for the treatment of COVID-19 as50 “unapproved new drugs sold in violation of section 505(a) of the Federal Food, Drug, and Cosmetic Act (FD&C Act), 2pt1 U.S.C. § 355(a).”
It’s ironic that Lurie offhandedly dismisses peer-reviewed published science51 that demonstrates your immune function is dependent on certain nutrients and they help to lower your risk of severe infection, whether it’s from COVID-19, the seasonal flu, the common cold or anything else.
Instead, he calls for mask-wearing52 that has no published scientific evidence to back universal use, as one of the most important prevention strategies against COVID-19. In a blog post, published May 18, 2021, he says, “… while mask relaxation may make sense for most of the vaccinated most of the time, it has the potential to destroy the social norm of mask wearing.”
CSPI Would Like to Censor Free Speech
I have been writing about the importance of vitamin D for your overall health for over a decade. Yet, the CSPI has chosen 2020 to censor my efforts to educate people on the importance of maintaining adequate vitamin D levels. In 2020, I co-wrote a paper with William Grant, Ph.D.,53 and Dr. Carol Wagner,54 both of whom are on the GrassrootsHealth vitamin D expert panel.55
The paper demonstrated the clear link that exists between vitamin D deficiency and severe cases of COVID-19. You can find the paper in the peer-reviewed medical journal Nutrients where it was published in October 2020.56
The FDA’s warning letter has highlighted statements in articles published on my website that are fully referenced, cited and supported by published science. I am committed to providing truthful information, for free, to anyone who wants it. I support having a rigorous scientific debate but cannot support unauthenticated and counterfeit accusations that fly in the face of published, peer-reviewed science.
It should never be a crime to report the findings of scientists and researchers. When censorship becomes the foundational method of influencing public opinion and health strategies, it is sure to lead down a disastrous road.
For the record, we have fully addressed the warning letter from the FDA. It is simply against the First Amendment of the U.S. Constitution for the FDA to stop free speech that the CSPI does not like.
CSPI Has Repeatedly Violated Its Mission Statement
This is not the first time that recommendations from the CSPI have endangered public health. In the past, CSPI described trans fats as “a great boon to American arteries”57 after heartily endorsing them years earlier by saying, “there is little good evidence that trans fats cause any more harm than other fats.”58
In the real world, this highly successful trans-fat campaign that began in 1986 resulted in an epidemic of heart disease. When the organization began reversing its decision on synthetic trans fats, it never admitted the error and simply switched the blame, erasing the previous pro-trans fat articles from its website and then posting a timeline59 on artificial trans fats that simply skips what they previously promoted.
The timeline begins in 1993 when CSPI “suddenly” decided to urge the FDA to label trans fats, and works up to 2003 when CSPI proudly says it took out a full-page ad in The New York Times “slamming McDonald’s for ‘Broken McPromise’ on trans fat.” This, despite the fact that in 198660 they criticized McDonald’s for not switching to trans fats sooner, like other fast-food restaurants already had.
While CSPI would prefer you to believe they’ve always been against trans fats, some people still remember what they and their officers said in the past, and comments their officers and members made when they switched their position have been preserved on others’ websites.
For example, Weston A. Price61 details how CSPI’s director of nutrition Bonnie Liebman changed her organization’s tune in December 1992, when she totally ignored CSPI’s support for trans fats only a few years earlier and blamed the margarine industry for promoting trans fats, writing:
“We’ve been crying ‘foul’ for some time now, as the margarine industry has tried to convince people that eating margarine was as good for their hearts as aerobic exercise … And we warned folks several years ago that trans fatty acids could be a problem.”
Continuing in their historical footsteps, the CSPI continues to recommend eating unsaturated fats like oil and canola oil,62 while avoiding butter and other healthy saturated fats, saying that “changing fats doesn’t lower the risk of dying.”63
Trans fats aren’t the only foods that CSPI made an about-face on something they’d promoted as healthy for years, however. It wasn’t until 2013 that CSPI downgraded the artificial sweetener Splenda from the “safe” category to “caution.”64 It took another three years to downgrade it again from “caution” to “avoid.”65
Yet, the organization continues to promote diet sodas as a safer alternative to regular soda, saying it “does not promote diabetes, weight gain or heart disease in the way that full calorie sodas do”66 — even though numerous peer-reviewed studies say otherwise.67,68,69
The CSPI’s support of suspected, and in some cases well verified, health hazards of trans fats, and artificial sweeteners, along with soy, GMOs, low-fat diets and fake meat, reveals that the intent of the organization to protect and advance public health is questionable to say the least.
The CSPI appears more interested in protecting profitable industries and their effort to destroy companies selling vitamins and supplements with natural antiviral effects is just more evidence of that.
Sources and References
- 1 Endotext January 19, 2018
- 2 NIH Vitamin D March 22, 2021
- 3 American Journal of Respiratory and Critical Care Medicine February 3, 20211
- 4 Int J Mol Sci. 2018 Aug; 19(8): 2419
- 5 Circulation Research January 17, 2014
- 6 Clinical Journal of the American Society of Nephrology September 2009
- 7 Europe PM January 1993
- 8 Frontiers in Physiology April 29, 2014
- 9 Brain Sciences September 2020
- 10 British Journal of Nutrition October 16, 2019
- 11 Clinical Nutrition ESPEN April 2021
- 12, 36 Journal of Infection and Public Health October 2020
- 13 Archives of Endocrinology and Metabolism September-October 2020
- 14, 16, 26 Health Security, 2021;19(3)
- 15, 29, 30 Trinity College Dublin, September 15, 2021
- 17 News Medical Life Sciences, Vitamin D Overdose
- 18 Medline Plus, Acetaminophen Overdose
- 19 Medscape, January 17, 2020
- 20 StatPearls Publishing, Acetaminophen Toxicity
- 21 Nutrients, 2018;10(8)
- 22 British Journal of Clinical Pharmacology, 2018;84(6)
- 23 Irish Journal of Medical Science, 2014;183(3)
- 24 Grassroots Health, May 28, 2019, top line
- 25 Nutrition Research, 2011;31(1)
- 27 Nutrients, 2020;12(4)
- 28 Health Security, 2021;19(3) Conclusion
- 31, 33 Scientific Reports, 2021;11(18262)
- 32 Biobank
- 34 European Journal of Clinical Nutrition, 2020;74
- 35 medRxiv, May 13, 2020; doi.org/10.1101/2020.05.08.20095893
- 37 JAMA Infectious Diseases, 2020;3(9)
- 38 Journal of Steroid and Biochemical Molecular Biology, 2020;204(105771)
- 39 Nutrients, 2020;12(9)
- 40 Medicine in Drug Discovery, 2020;7(100051)
- 41, 44 CSPInet.org July 21, 2020
- 42 Common Dreams, January 7, 2019
- 43 Influence Watch, Center for Science in the Public Interest (CSPI)
- 45 CSPInet.org Appendix of Illegal Claims
- 46 CSPInet.org July 19, 2017
- 47 CSPInet.org Peter Lurie Bio
- 48, 50 FDA.gov Mercola.com warning letter February 18, 2021
- 49 CSPInet.org, March 4, 2021
- 51 KOMO News, November 4, 2020
- 52 CSPInet.org, May 18, 2021
- 53 SUNARC.org William Grant Bio
- 54 MUSC Carol Wagner MD Bio
- 55 GrassrootsHealth Expert Panel
- 56 Nutrients, 2020;12(11)
- 57 The Atlantic November 8, 2013
- 58 CSPInet.org, The Truth About Trans Fats March 1988
- 59 CSPInet.org Trans Fat Timeline
- 60 Research Gate January 2012
- 61 Weston A Price January 6, 2003
- 62 CSPInet.org Canola Oil
- 63 CSPInet.org Big Fat Myths
- 64 CSPInet.org June 12, 2013
- 65 CSPInet.org February 8, 2016
- 66 CSPInet.org Sugary Drinks 70% down the page, What can you do?
- 67 Journal of the American Geriatrics Society March 17, 2015
- 68 Eur J Clin Nutr. 2020 Feb; 74(2): 322–327
- 69 Food Research International February 18, 2021
October 5, 2021 Posted by aletho | Civil Liberties, Deception, Full Spectrum Dominance, Timeless or most popular | Center for Science in the Public Interest, Covid-19, COVID-19 Vaccine, Vitamin D | Leave a comment
APOE-4: The Clue to Why Low Fat Diet and Statins may Cause Alzheimer’s
By Dr. Stephanie Seneff | December 15, 2009
Abstract
Alzheimer’s is a devastating disease whose incidence is clearly on the rise in America. Fortunately, a significant number of research dollars are currently being spent to try to understand what causes Alzheimer’s. ApoE-4, a particular allele of the apolipoprotein apoE, is a known risk factor. Since apoE plays a critical role in the transport of cholesterol and fats to the brain, it can be hypothesized that insufficient fat and cholesterol in the brain play a critical role in the disease process. In a remarkable recent study, it was found that Alzheimer’s patients have only 1/6 of the concentration of free fatty acids in the cerebrospinal fluid compared to individuals without Alzheimer’s. In parallel, it is becoming very clear that cholesterol is pervasive in the brain, and that it plays a critical role both in nerve transport in the synapse and in maintaining the health of the myelin sheath coating nerve fibers. An extremely high-fat (ketogenic) diet has been found to improve cognitive ability in Alzheimer’s patients. These and other observations described below lead me to conclude that both a low-fat diet and statin drug treatment increase susceptibility to Alzheimer’s.
1. Introduction
Alzheimer’s is a devastating disease that takes away the mind bit by bit over a period of decades. It begins as odd memory gaps but then steadily erodes your life to the point where around-the-clock care is the only option. With severe Alzheimer’s, you can easily wander off and get lost, and may not even recognize your own daughter. Alzheimer’s was a little known disease before 1960, but today it threatens to completely derail the health system in the United States.
Currently, over 5 million people in America have Alzheimer’s. On average, a person over 65 with Alzheimer’s costs three times as much for health care as one without Alzheimer’s. More alarmingly, the incidence of Alzheimer’s is on the rise. Dr. Murray Waldman has studied epidemiological data comparing Alzheimer’s with femur fractures, looking back over the last fifty years [52]. Alarmingly, he has found that, while the incidence of femur fractures (another condition which typically increases with age) has gone up only at a linear rate, the increase in the incidence of Alzheimer’s has gone up exponentially, between 1960 and 2010 Alzheimer’s Epidemic [15]. Just between 2000 and 2006, US Alzheimer’s deaths rose by 47%, while, by comparison, deaths from heart disease, breast cancer, prostate cancer, and stroke combined decreased by 11%. This increase goes far beyond people living longer: for people 85 and older, the percentage who died from Alzheimer’s rose by 30% between 2000 and 2005 [2]. Finally, it’s likely these are under-estimates, as many people suffering with Alzheimer’s ultimately die of something else. You likely have a close friend or relative who is suffering from Alzheimer’s.
Something in our current lifestyle is increasing the likelihood that we will succumb to Alzheimer’s. My belief is that two major contributors are our current obsession with low-fat diet, combined with the ever expanding use of statin drugs. I have argued elsewhere that low-fat diet may be a major factor in the alarming increase in autism and adhd in children. I have also argued that the obesity epidemic and the associated metabolic syndrome can be traced to excessive low-fat diet. Statins are likely contributing to an increase in many serious health issues besides Alzheimer’s, such as sepsis, heart failure, fetal damage, and cancer, as I have argued here. I believe the trends will only get worse in the future, unless we substantially alter our current view of “healthy living.”
The ideas developed in this essay are the result of extensive on-line research I conducted to try to understand the process by which Alzheimer’s develops. Fortunately, a great deal of research money is currently being spent on Alzheimer’s, but a clearly articulated cause is still elusive. However, many exciting leads are fresh off the press, and the puzzle pieces are beginning to assemble themselves into a coherent story. Researchers are only recently discovering that both fat and cholesterol are severly deficient in the Alzheimer’s brain. It turns out that fat and cholesterol are both vital nutrients in the brain. The brain contains only 2% of the body’s mass, but 25% of the total cholesterol. Cholesterol is essential both in transmitting nerve signals and in fighting off infections.
A crucial piece of the puzzle is a genetic marker that predisposes people to Alzheimer’s, termed “apoE-4.” ApoE plays a central role in the transport of fats and cholesterol. There are currently five known distinct variants of apoE (properly termed “alleles”), with the ones labelled “2”, “3” and “4” being the most prevalent. ApoE-2 has been shown to afford some protection against Alzheimer’s; apoE-3 is the most common “default” allele, and apoE-4, present in 13-15% of the population, is the allele that is associated with increased risk to Alzheimer’s. A person with apoE-4 allele inherited from both their mother and their father has up to a twenty-fold increased likelihood of developing Alzheimer’s disease. However, only about 5% of the people with Alzheimer’s actually have the apoE-4 allele, so clearly there is something else going on for the rest of them. Nonetheless, understanding apoE’s many roles in the body was a key step leading to my proposed low fat/statin theory.
2. Background: Brain Biology 101
Although I have tried to write this essay in a way that is accessible to the non-expert, it will still be helpful to first familiarize you with basic knowledge of the structure of the brain and the roles played by different cell types within the brain.
At the simplest level, the brain can be characterized as consisting of two major components: the gray matter and the white matter. The gray matter comprises the bodies of the neurons, including the cell nucleus, and the white matter contains the myriad of “wires” that connect each neuron to every other neuron it communicates with. The wires are known as “axons” and they can be quite long, connecting, for example, neurons in the frontal cortex (above the eyes) with other neurons deep in the interior of the brain concerned with memory and movement. The axons will figure prominently in the discussions below, because they are coated with a fatty substance called the myelin sheath, and this insulating layer is known to be defective in Alzheimer’s. Neurons pick up signals transmitted through the axons at junctures known as synapses. Here the message needs to be transmitted from one neuron to another one, and various neurotransmitters such as dopamine and GABA exert excitatory or inhibitory influences on signal strength. In adidtion to a single axon, neurons typically have several much shorter nerve fibers called dendrites, whose job is to receive incoming signals from diverse sources. At a given point in time, signals received from multiple sources are integrated in the cell body and a decision is made as to whether the accumulated signal strength is above threshold, in which case the neuron responds by firing a sequence of electrical pulses, which are then transmitted through the axon to a possibly distant destination.
In addition to the neurons, the brain also contains a large number of “helper” cells called glial cells, which are concerned with the care and feeding of neurons. Three principle types of glial cells will play a role in our later discussion: the microglia, the astrocytes, and the oligodendrocytes. Microglia are the equivalent of white blood cells in the rest of the body. They are concerned with fighting off infective agents such as bacteria and viruses, and they also monitor neuron health, making life-and-death decisions: programming a particular neuron for apoptosis (intentional self-destruction) if it appears to be malfunctioning beyond hope of recovery, or is infected with an organism that is too dangerous to let flourish.
The astrocytes figure very prominently in our story below. They nestle up against the neurons and are responsible for assuring an adequate supply of nutrients. Studies on neuron cultures from rodent central nervous systems have shown that neurons depend upon astrocytes for their supply of cholesterol [40]. Neurons critically need cholesterol, both in the synapse [50] and in the myelin sheath [45], in order to successfully transmit their signals, and also as a first line of defense against invasive microbes. Cholesterol is so important to the brain that astrocytes are able to synthesize it from basic ingredients, a skill not found in most cell types. They also supply the neurons with fatty acids, and they are able to take in short chain fatty acids and combine them to form the longer-chain types of fatty acids that are especially prominent in the brain [7][24][36], and then deliver them to neighboring neurons and to the cerebrospinal fluid.
The third type of glial cell is the oligodendrocyte. These cells specialize in making sure the myelin sheath is healthy. Oligodentrocytes synthesize a special sulfur-containing fatty acid, known as sulfatide, from other fatty acids supplied to them by the cerebrospinal fluid [9]. Sulfatide has been shown to be essential for the maintenance of the myelin sheath. Children born with a defect in the ability to metabolize sulfatide suffer from progressive demyelination, and rapid loss of motor and cognitive functions, resulting in an early death before the age of 5 [29]. Depletion in sulfatide is a well-known characterization of Alzheimer’s, even in early stages before it has been manifested as cognitive decline [18]. And ApoE has been shown to play a crucial role in the maintenance of sulfatide [19]. Throughout a person’s life, the myelin sheath has to be constantly maintained and repaired. This is something that researchers are only beginning to appreciate, but two related properties of Alzheimer’s are poor quality myelin sheath alongside a drastically reduced concentration of fatty acids and cholesterol in the cerebrospinal fluid [38].
3. Cholesterol and Lipid Management
In addition to some knowledge about the brain, you will also need to know something about the processes that deliver fats and cholesterol to all the tissues of the body, with a special focus on the brain. Most cell types can use either fats or glucose (a simple sugar derived from carbohydrates) as a fuel source to satisfy their energy needs. However, the brain is the one huge exception to this rule. All cells in the brain, both the neurons and the glial cells, are unable to utilize fats for fuel. This is likely because fats are too precious to the brain. The myelin sheath requires a constant supply of high quality fat to insulate and protect the enclosed axons. Since the brain needs its fats to survive long-term, it is paramount to protect them from oxidation (by exposure to oxygen) and from attack by invasive microbes.
Fats come in all kinds of shapes and sizes. One dimension is the degree of saturation, which concerns how many double bonds they possess, with saturated fats possessing none, monounsaturated fats having only one, and polyunsaturated fats having two or more. Oxygen breaks the double bond and leaves the fat oxidized, which is problematic for the brain. Polyunsaturated fats are thus the most vulnerable to oxygen exposure, because of multiple double bonds.
Fats are digested in the intestine and released into the blood stream in the form of a relatively large ball with a protective protein coat, called a chylomicron. The chylomicron can directly provide fuel to many cell types, but it may also be sent to the liver where the contained fats are sorted out and redistributed into much smaller particles, which also contain substantial amounts of cholesterol. These particles are called “lipoproteins,” (henceforth, LPP’s) because they contain protein in the spherical shell and lipids (fats) in the interior. If you’ve had your cholesterol measured, you’ve probably heard of LDL (low density LPP) and HDL (high density LPP). If you think these are two different kinds of cholesterol, you would be mistaken. They are just two different kinds of containers for cholesterol and fats that serve different roles in the body. There are actually several other LPP’s, for example, VLDL (very-low) and IDL (intermediate), as shown in the accompanying diagram. 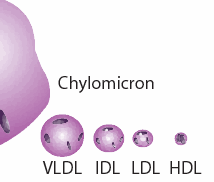 In this essay I will refer to these collectively as the XDL’s. As if this weren’t confusing enough, there is also another unique XDL that is found only in the cerebrospinal fluid, that supplies the nutritional needs of the brain and nervous system. This one doesn’t seem to have a name yet, but I will call it “B-HDL,” because it is like HDL in terms of its size, and “B” is for “brain [13]”
In this essay I will refer to these collectively as the XDL’s. As if this weren’t confusing enough, there is also another unique XDL that is found only in the cerebrospinal fluid, that supplies the nutritional needs of the brain and nervous system. This one doesn’t seem to have a name yet, but I will call it “B-HDL,” because it is like HDL in terms of its size, and “B” is for “brain [13]”
An important point about all the XDL’s is that they contain distinctly different compositions, and each is targeted (programmed) for specific tissues. A set of proteins called “apolipoproteins” or, equivalently, “apoproteins” (“apo’s” for short) figure strongly in controlling who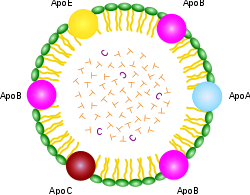 gets what. As you can see from the schematic of the chylomicron shown at the right, it contains a rainbow of different apo’s for every conceivable application. But the XDL’s are far more specific, with HDL containing “A,” LDL containing “B,” VLDL containing “B” and “C,” and IDL containing only “E.” The apo’s have special binding properties that allow the lipid contents to be transported across cell membranes so that the cell can gain access to the fats and choleseterol contained inside.
gets what. As you can see from the schematic of the chylomicron shown at the right, it contains a rainbow of different apo’s for every conceivable application. But the XDL’s are far more specific, with HDL containing “A,” LDL containing “B,” VLDL containing “B” and “C,” and IDL containing only “E.” The apo’s have special binding properties that allow the lipid contents to be transported across cell membranes so that the cell can gain access to the fats and choleseterol contained inside.
The only apo that is of concern to us in the context of this essay is apoE. ApoE is very important to our story because of its known link with Alzheimer’s disease. ApoE is a protein, i.e., sequence of amino acids, and its specific composition is dictated by a corresponding DNA sequence on a protein-coding gene. Certain alterations in the DNA code lead to defects in the ability of the transcribed protein to perform its biological roles. ApoE-4, the allele associated with increased risk to Alzheimer’s, is presumably unable to perform its tasks as efficiently as the other alleles. By understanding what apoE does, we can better infer how the consequences of doing it poorly might impact the brain, and then observe experimentally whether the features of the Alzheimer’s brain are consistent with the roles played by apoE.
A strong clue about apoE’s roles can be deduced from where it is found. As I mentioned above, it is the only apo in both B-HDL in the cerebrospinal fluid and IDL in the blood serum. Only selected cell types can synthesize it, the two most significant of which for our purposes are the liver and the astrocytes in the brain. Thus the astrocytes provide the linkage between the blood and the cerebrospinal fluid. They can usher lipids and cholesterol across the blood-brain barrier, via the special key which is apoE.
It turns out that, although apoE is not found in LDL, it does bind to LDL, and this means that astrocytes can unlock the key to LDL in the same way that they can gain access to IDL, and hence the cholesterol and fatty acid contents of LDL are accessible to astrocytes as well, as long as apoE is functioning properly. The astrocytes reshape and repackage the lipids and release them into the cerebospinal fluid, both as B-HDL and simply as free fatty acids, available for uptake by all parts of the brain and nervous system [13].
One of the critical reshaping steps is to convert the fats into types that are more attractive to the brain. To understand this process you need to know about another dimension of fats besides their degree of saturation, which is their total length. Fats have a chain of linked carbon atoms as their spine, and the total number of carbons in a particular fat characterizes it as short, medium length, or long. The brain works best when the constituent fats are long, and, indeed, the astrocytes are able to take in short chain fats and reorganize them to make longer chain fats [24].
A final dimension of fats that plays a role is where the first double bond is located in a polyunsaturated fat, which distinguishes omega-3 from omega-6 fats (position 3; position 6). Omega-3 fats are very common in the brain. Certain ones of the omega-3 and omega-6 fats are essential fatty acids, in that the human body is unable to synthesize them, and therefore depends upon their supply from the diet. This is why it is claimed that fish “makes you smart”: because cold water fish is the best source of essential omega-3 fats.
Now I want to return to the subject of the XDL’s. It is a dangerous journey from the liver to the brain, as both oxygen and microbes are found in abundance in the blood stream. The XDL’s protective shell contains both LPP’s andunesterified cholesterol, as well as the signature apo that controls which cells can receive the contents, as shown in the accompanying schematic. 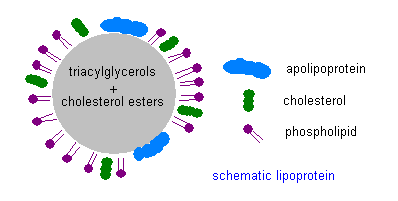 The internal contents are esterified cholesterol and fatty acids, along with certain antioxidants that are conveniently being transported to the cells packaged in the same cargo ship. Esterification is a technique to render the fats and cholesterol inert, which helps protect them from oxidation [51]. Having the antioxidants (such as vitamin E and Coenzyme Q10) along for the ride is also convenient, as they too protect against oxidation. The cholesterol contained in the shell, however, is intentionally not esterified, which means that it is active. One of its roles there is to guard against invasive bacteria and viruses [55]. Cholesterol is the first line of defense against these microbes, as it will alert the white blood cells to attack whenever it encounters dangerous pathogens. It has also been proposed that the cholesterol in the XDL’s shell itself acts as an antioxidant [48].
The internal contents are esterified cholesterol and fatty acids, along with certain antioxidants that are conveniently being transported to the cells packaged in the same cargo ship. Esterification is a technique to render the fats and cholesterol inert, which helps protect them from oxidation [51]. Having the antioxidants (such as vitamin E and Coenzyme Q10) along for the ride is also convenient, as they too protect against oxidation. The cholesterol contained in the shell, however, is intentionally not esterified, which means that it is active. One of its roles there is to guard against invasive bacteria and viruses [55]. Cholesterol is the first line of defense against these microbes, as it will alert the white blood cells to attack whenever it encounters dangerous pathogens. It has also been proposed that the cholesterol in the XDL’s shell itself acts as an antioxidant [48].
HDL’s are mostly depleted of the lipid and cholesterol content, and they are tasked with returning the empty shell back to the liver. Once there, cholesterol will be recommissioned to enter the digestive system as part of the bile, which is produced by the gall bladder to help digest ingested fats. But the body is very careful to conserve cholesterol, so that 90% of it will be recycled from the gut back into the blood stream, contained in the chylomicron that began our story about fats.
In summary, the management of the distribution of fats and cholesterol to the cells of the body is a complex process, carefully orchestrated to assure that they will have a safe journey to their destination. Dangers lurk in the blood stream, mostly in the form of oxygen and invasive microbes. The body considers cholesterol to be precious cargo, and it is very careful to conserve it, by recycling it from the gut back to the liver, to be appropriately distributed among the XDL’s that will deliver both cholesterol and fats to the tissues that depend upon them, most especially the brain and nervous system.
4. The Relationship between Cholesterol and Alzheimer’s
Through retrospective studies, the statin industry has been very successful at the game of pretending that benefits derived from high cholesterol are actually due to statins, as I have described at length in an essay on the relationship between statins and fetal damage, sepsis, cancer, and heart failure. In the case of Alzheimer’s, they are playing this game in reverse: they are blaming cholesterol for a very serious problem that I believe is actually caused by statins.
The statin industry has looked long and hard for evidence that high cholesterol might be a risk factor for Alzheimer’s. They examined cholesterol levels for men and women of all ages between 50 and 100, looking back 30 or more years if necesssary, to see if there was ever a correlation between high cholesterol and Alzheimer’s. They found only one statistically significant relationship: men who had had high cholesterol in their 50’s had an increased susceptibility to Alzheimer’s much later in life [3].
The statin industry has jumped on this opportunity to imply that high cholesterol might cause Alzheimer’s, and, indeed, they have been very fortunate in that reporters have taken the bait and are promoting the idea that, if high cholesterol many years ago is linked to Alzheimer’s, then statins might protect from Alzheimer’s. Fortunately, there exist lengthy web pages (Cholesterol Doesn’t Cause Alzheimer’s) that have documented the long list of reasons why this idea is absurd.
Men who have high cholesterol in their 50’s are the poster child for statin treatment: all of the studies that have shown a benefit for statins in terms of reducing the number of minor heart attacks involved men in their 50’s. High cholesterol is positively correlated with longevity in people over 85 years old [54], and has been shown to be associated with better memory function [53] and reduced dementia [35]. The converse is also true: a correlation between falling cholesterol levels and Alzheimer’s [39]. As will be discussed further later, people with Alzheimer’s also have reduced levels of B-HDL, as well as sharply reduced levels of fatty acids, in the cerbrospinal fluid, i.e, impoverished supply of cholesterol and fats to the myelin sheath [38]. As we saw earlier, fatty acid supply is essential as building blocks for the sulfatide that is synthesized by oligodendrocytes to keep the myelin sheath healthy [29].
The obvious study that needs to be done is to bin the men who had high cholesterol in their 50’s into three groups: those who never took statins, those who took smaller doses for shorter times, and those who took larger doses for longer times. Such a study would not be hard to do; in fact, I suspect something like it has already been done. But you’ll never hear about it because the statin industry has buried the results.
In a very long term retrospective cohort study of members of the Permanente Medical Care Program in northern California, researchers looked at cholesterol data that were obtained between 1964 and 1973 [46]. They studied nearly ten thousand people who had remained members of that health plan in 1994, upon the release of computerized outpatient diagnoses of dementia (both Alzheimer’s and vascular dementia). The subjects were between 40 and 45 years old when the cholesterol data were collected.
The researchers found a barely statistically significant result that people who were diagnosed with Alzheimer’s had higher cholesterol in their 50’s than the control group. The mean value for the Alzheimer’s patients was 228.5, as against 224.1 for the controls.
The question that everybody ought to be asking is: for the Alzheimer’s group, how did the people who later took statins stack up against the people who didn’t? In extreme understatement, the authors offhandedly remark in the middle of a paragraph: “Information on lipid-lowering treatments, which have been suggested to decrease dementia risk [31], was not available for this study.” You can be sure that, if there was any inkling that the statins might have helped, these researchers would have been allowed access to those data.
The article they refer to for support, reference [19] in [46] (which is reference [44] here) was very weak. The abstract for that article is repeated in full here in the Appendix. But the concluding sentence sums it up well: “A more than a modest role for statins in preventing AD [Alzheimer’s Disease] seems unlikely.” This is the best they can come up with to defend the position that statins might protect from Alzheimer’s.
An intuitive explanation for why high cholesterol at an early age might be correlated with Alzheimer’s risk has to do with apoE-4. People with that allele are known to have high cholesterol early in life [39], and I believe this is a protective strategy on the part of the body. The apoE-4 allele is likely defective in the task of importing cholesterol into the astrocytes, and therefore an increase in the bioavailability of cholesterol in blood serum would help to offset this deficit. Taking a statin would be the last thing a person in that situation would want to do.
5. Do Statins Cause Alzheimer’s?
There is a clear reason why statins would promote Alzheimer’s. They cripple the liver’s ability to synthesize cholesterol, and as a consequence the level of LDL in the blood plummets. Cholesterol plays a crucial role in the brain, both in terms of enabling signal transport across the synapse [50] and in terms of encouraging the growth of neurons through healthy development of the myelin sheath [45]. Nonetheless, the statin industry proudly boasts that statins are effective at interfering with cholesterol production in the brain [31][47] as well as in the liver.
Yeon-Kyun Shin is an expert on the physical mechanism of cholesterol in the synapse to promote transmission of neural messages, and one of the authors of [50] referenced earlier. In an interview by a Science Daily reporter, Shin said: “If you deprive cholesterol from the brain, then you directly affect the machinery that triggers the release of neurotransmitters. Neurotransmitters affect the data-processing and memory functions. In other words — how smart you are and how well you remember things.”
A recent review of two large population-based double-blind placebo-controlled studies of statin medications in individuals at risk for dementia and Alzheimer disease showed that statins are not protective against Alzheimer’s [34]. The lead author of the study, Bernadette McGuinness, was quoted by a reporter from Science Daily as saying, “From these trials, which contained very large numbers and were the gold standard — it appears that statins given in late life to individuals at risk of vascular disease do not prevent against dementia.” A researcher at UCLA, Beatrice Golomb, when asked to comment on the results, was even more negative, saying, “Regarding statins as preventive medicines, there are a number of individual cases in case reports and case series where cognition is clearly and reproducibly adversely affected by statins.” In the interview, Golomb remarked that various randomized trials have shown that statins were either adverse or neutral towards cognition, but none have shown a favorable response.
A common side effect of statins is memory dysfunction. Dr. Duane Graveline, fondly known as “spacedoc” because he served as a doctor to the astronauts, has been a strong advocate against statins and is collecting evidence of statin side effects directly from statin users around the world. He was led to this assault on statins as a consequence of his own personal experience of transient global amnesia, a frightening episode of total memory loss which he is convinced was caused by the statin drugs he was taking at the time. He has now completed three books describing a diverse collection of damning side effects of statins, the most famous of which is Lipitor: Thief of Memory [17].
A second way (besides their direct impact on cholesterol) in which statins likely impact Alzheimer’s is in their indirect negative effect on the supply of fatty acids and antioxidants to the brain. It is a given that statins drastically reduce the level of LDL in the blood serum. This is their claim to fame. It is interesting, however, that they succeed in reducing not just the amount of cholesterol contained in the LDL particles, but rather the actual number of LDL particles altogether. This means that, in addition to depleting cholesterol, they reduce the available supply to the brain of both fatty acids and antixodiants, which are also carried in the LDL particles. As we’ve seen, all three of these substances are essential to proper brain functioning.
I conjecture that the reasons for this indirect effect are two-fold: (1) there is inadequate cholesterol in the bile to metabolize dietary fats, and (2) the rate-limiting effect on the production of LDL is the ability to provide adequate cholesterol in the shell to assure survival of the contents during transport in the blood stream; i.e., to protect the contents from oxidation and marauding bacteria and viruses. People who take the highest 80 mg/dl dosage of statins often end up with LDL levels as low as 40mg/dl, well below even the lowest numbers observed naturally. I shudder to think of the probable long-term consequences of such severe depletion in fats, cholesterol, and antioxidants.
A third way in which statins may promote Alzheimer’s is by crippling the ability for cells to synthesize coenzyme Q10. Coenzyme Q10 has the misfortune of sharing the same metabolic pathway as cholesterol. Statins interfere with a crucial intermediate step on the pathway to the synthesis of both cholesterol and coenzyme Q10. Coenzyme Q10 is also known as “ubiquinone” because it seems to show up everywhere in cell metabolism. It is found both in the mitochondria and in the lysosomes, and its critical role in both places is as an antioxidant. The inert esters of both cholesterol and fatty acids are hydrolyzed and activated in the lysosomes [8], and then released into the cytoplasm. Coenzyme Q10 consumes excess oxygen to keep it from doing oxidative damage [30], while also generating energy in the form of ATP (adenosine triphosphate, the universal energy currency in biology).
The final way in which statins should increase Alzheimer’s risk is through their indirect effect on vitamin D. 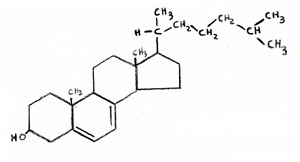 Vitamin D is synthesized from cholesterol in the skin, upon exposure to UV rays from the sun. In fact, the chemical formula of vitamin D is almost indistinguishable from that of cholesterol, as shown in the two attached figures (cholesterol on the left, vitamin D on the right). If LDL levels are
Vitamin D is synthesized from cholesterol in the skin, upon exposure to UV rays from the sun. In fact, the chemical formula of vitamin D is almost indistinguishable from that of cholesterol, as shown in the two attached figures (cholesterol on the left, vitamin D on the right). If LDL levels are 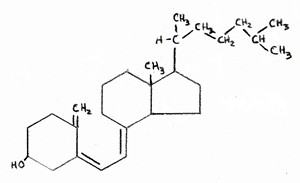 kept artificially low, then the body will be unable to resupply adequate amounts of cholesterol to replenish the stores in the skin once they have been depleted. This would lead to vitamin D deficiency, which is a widespread problem in America.
kept artificially low, then the body will be unable to resupply adequate amounts of cholesterol to replenish the stores in the skin once they have been depleted. This would lead to vitamin D deficiency, which is a widespread problem in America.
It is well known that vitamin D fights infection. To quote from [25], “Patients with severe infections as in sepsis have a high prevalence of vitamin D deficiency and high mortality rates.” As will be elaborated on later, a large number of infective agents have been shown to be present in abnormally high amounts in the brains of Alzheimers patients [27][26].
Dr. Grant has recently argued [16] that there are many lines of evidence pointing to the idea that dementia is associated with vitamin D deficiency. An indirect argument is that vitamin D deficiency is associated with many conditions that in turn carry increased risk for dementia, such as diabetes, depression, osteoporosis, and cardiovascular disease. Vitamin D receptors are widespread in the brain, and it is likely that they play a role there in fighting off infection. Vitamin D surely plays other vital roles in the brain as well, as powerfully suggested by this quote taken from the abstract of [32]: “We conclude there is ample biological evidence to suggest an important role for vitamin D in brain development and function.”
6. Astrocytes, Glucose Metabolism, and Oxygen
Alzheimer’s is clearly correlated with a deficiency in the supply of fat and cholesterol to the brain. IDL, when functioning properly, is actually incredibly efficient in cholesterol and fat throughput from the blood across cell membranes, compared to LDL [8]. It gives up its contents much more readily than the other apo’s. And it achieves this as a direct consequence of apoE. IDL (as well as LDL) in the blood delivers fats and cholesterol to the astrocytes in the brain, and the astrocytes can thus use this external source instead of having to produce these nutrients themselves. I suspect, in fact, that astrocytes only produce a private supply when the external supply is insufficient, and they do so reluctantly.
Why would it be disadvantageous for an astrocyte to synthesize its own fats and cholesterol? In my opinion, the answer has to do with oxygen. An astrocyte needs a significant energy source to synthesize fats and cholesterol, and this energy is usually supplied by glucose from the blood stream. Furthermore, the end-product of glucose metabolism is acetyl-Coenzyme A, the precursor to both fatty acids and cholesterol. Glucose can be consumed very efficiently in the mitochondria, internal structures within the cell cytoplasm, via aerobic processes that require oxygen. The glucose is broken down to produce acetyl-Coenzyme A as an end-product, as well as ATP, the source of energy in all cells.
However, oxygen is toxic to lipids (fats), because it oxidizes them and makes them rancid. Lipids are fragile if not encased in a protective shell like IDL, HDL, or LDL. Once they are rancid they are susceptible to infection by invasive agents like bacteria and viruses. So an astrocyte trying to synthesize a lipid has to be very careful to keep oxygen out, yet oxygen is needed for efficient metabolism of glucose, which will provide both the fuel (ATP) and the raw materials (acetyl-Coenzyme A) for fat and cholesterol synthesis.
What to do? Well, it turns out that there is an alternative, although much less efficient, solution: to metabolize glucose anaerobically directly in the cytoplasm. This process does not depend on oxygen (a great advantage) but it also yields substantially less ATP (only 6 ATP as contrasted with 30 if glucose is metabolized aerobically in the mitochondria). The end product of this anaerobic step is a substance called pyruvate, which could be further broken down to yield a lot more energy, but this process is not accessible to all cells, and it turns out that the astrocytes need help for this to happen, which is where amyloid-beta comes in.
7. The Crucial Role of Amyloid-Beta
Amyloid-beta (also known as “abeta”) is the substance that forms the famous plaque that accumulates in the brains of Alzheimer’s patients. It has been believed by many (but not all) in the research community that amyloid-beta is the principal cause of Alzheimer’s, and as a consequence, researchers are actively seeking drugs that might destroy it. However, amyloid-beta has the unique capability of stimulating the production of an enzyme, lactate dehydrogenase, which promotes the breakdown of pyruvate (the product of anaerobic glucose metabolism) into lactate, through an anaerobic fermentation process, with the further production of a substantial amount of ATP.
The lactate, in turn, can be utilized itself as an energy source by some cells, and it has been established that neurons are on the short list of cell types that can metabolize lactate. So I conjecture that the lactate is transported from the astrocyte to a neighboring neuron to enhance its energy supply, thus reducing its dependence on glucose. It is also known that apoE can signal the production of amyloid-beta, but only under certain poorly understood environmental conditions. I suggest those environmental triggers have to do with the internal manufacture of fats and cholesterol as opposed to the extraction of these nutrients from the blood supply. I.e., amyloid-beta is produced as a consequence of environmental oxidative stress due to an inadequate supply of fats and cholesterol from the blood.
In addition to being utilized as an energy source by being broken down to lactate, pyruvate can also be used as a basic building block for synthesizing fatty acids. So anaerobic glucose metabolism, which yields pyruvate, is a win-win-win situation: (1) it significantly reduces the risk of exposure of fatty acids to oxygen, (2) it provides a source of fuel for neighboring neurons in the form of lactate, and (3) it provides a basic building block for fatty acid synthesis. But it depends upon amyloid-beta to work.
Thus, in my view (and in the view of others [28] [20] Amyloid-Beta and Alzheimer’s), amyloid-beta is not a cause of Alzheimer’s, but rather a protective device against it. The abstract of reference [28] arguing this point of view is reproduced in full in the Appendix. Several variants of a genetic defect associated with amyloid precursor protein (APP), the protein from which amyloid-beta is derived, have now been identified. A defect in this protein, which is associated with an increased risk of early onset Alzheimer’s, would likely lead to a reduced ability to synthesize amyloid-beta, which would then leave the brain with a big problem, since both the fuel and the basic building blocks for fatty acid synthesis would be in short supply, while oxygen trekking through the cell to the mitochondria would be exposing whatever fats were being synthesized to oxidation. The cell would likely be unable to keep up with need, and this would lead to a reduction in the number of fatty acids in the Alzheimer’s cerebrospinal fluid, a well-established characteristic of Alzheimer’s [38].
8. Cholesterol’s Role in the Brain
The brain comprises only 2% of the body’s total weight, yet it contains nearly 25% of the total cholesterol in the body. It has been determined that the limiting factor allowing the growth of synapses is the availability of cholesterol, supplied by the astrocytes. Cholesterol plays an incredibly important role in the synapse, by shaping the two cell membranes into a snug fit so that the signal can easily jump across the synapse [50]. So inadequate cholesterol in the synapse will weaken the signal at the outset, and inadequate fat coating the myelin sheath will further weaken it and slow it down during transport. A neuron that can’t send its messages is a useless neuron, and it only makes sense to prune it away and scavenge its contents.
The neurons that are damaged in Alzheimer’s are located in specific regions of the brain associated with memory and high level planning. These neurons need to transmit signals long distances between the frontal and prefrontal cortex and the hippocampus, housed in the midbrain. The transport of these signals depends on a strong and tight connection in the synapse, where the signal is transferred from one neuron to another, and a secure transmission across the long nerve fiber, a part of the white matter. The myelin sheath which coats the nerve fiber consists mainly of fatty acids, along with a substantial concentration of cholesterol. If it is not well insulated, the signal transmission rate will slow down and the signal strength will be severely reduced. Cholesterol is crucial for the myelin as well as for the synapse, as demonstrated dramatically through experiments conducted on genetically defective mice by Gesine Saher et al. [45]. These mutant mice lacked the ability to synthesize cholesterol in myelin-forming oligodendrocytes. They had severly disturbed myelin in their brains, and exhibited ataxia (uncoordinated muscle movements) and tremor. In the abstract, the authors wrote unequivocally, “This shows that cholesterol is an indispensable component of myelin membranes.”
In a post-mortem study comparing Alzheimer’s patients with a control group without Alzheimer’s, it was found that the Alzheimer’s patients had significantly reduced amounts of cholesterol, phospholipids (e.g, B-HDL), and free fatty acids in the cerebrospinal fluid than did the controls [38]. This was true irrespective of whether the Alzheimer’s patients were typed as apoE-4. In other words, reductions in these critical nutrients in the spinal fluid are associated with Alzheimer’s regardless of whether the reduction is due to defective apoE. The reductions in fatty acids were alarming: 4.5 micromol/L in the Alzheimer’s patients, compared with 28.0 micromol/L in the control group. This is a reduction by more than a factor of 6 in the amount of fatty acid available to repair the myelin sheath!
People with the apoE-4 allele tend to have high serum cholesterol. The question of whether this high cholesterol level might be an attempt on the part of the body to adjust for a poor rate of cholesterol uptake in the brain was addressed by a team of researchers in 1998 [39]. They studied 444 men between 70 and 89 years old at the time, for whom there existed extensive records of cholesterol levels dating back to several decades ago. Most significantly, cholesterol levels fell for the men who developed Alzheimer’s prior to their showing Alzheimer’s symptoms. The authors suggested that their high cholesterol might have been a protective mechanism against Alzheimer’s.
One might wonder why their cholesterol levels fell. There was no mention of statin drugs in the article, but statins would certainly be an effective way to reduce cholesterol levels. The statin industry would like people to believe that high cholesterol is a risk factor for Alzheimer’s, and they are quite thrilled that high cholesterol early in life is correlated with Alzheimer’s much later. But these results suggest quite the opposite: that blood cholesterol levels are kept high intentionally by the body regulatory mechanisms in an attempt to compensate for the defect. A high concentration will lead to an increase in the rate of delivery to the brain, where it is critically needed to keep the myelin sheath healthy and to promote neuron signaling in the synapses.
Using MRI technology, researchers at UCLA were able to measure the degree of breakdown of myelin in specific regions of the brain [6]. They conducted their studies on over 100 people between 55 and 75 years old, for whom they also determined the associated apoE allele (2, 3, or 4). They found a consistent trend in that apoE-2 had the least amount of degradation, and apoE-4 had the most, in the frontal lobe region of the brain. All of the people in the study were thus far healthy with respect to Alzheimer’s. These results show that premature breakdown of myelin sheath (likely due to an insufficient supply of fats and cholesterol to repair it) is associated with apoE-4.
To summarize, I hypothesize that, for the apoE-4 Alzheimer’s patients, defective apoE has led to an impaired ability to transport fats and cholesterol from the blood stream, via the astrocytes, into the cerebrospinal fluid. The associated high blood serum cholesterol is an attempt to partially correct for this defect. For the rest of the Alzheimer’s patients (the ones without the apoE-4 allele but who also have severely depleted fatty acids in their cerebrospinal fluid), we have to look for another reason why their fatty acid supply chain might be broken.
9. Infections and Inflammation
To summarize what I have said so far, Alzheimer’s appears to be a consequence of an inability of neurons to function properly, due to a deficiency in fats and cholesterol. A compounding problem is that the fats over time will become rancid if they cannot be adequately replenished. Rancid fats are vulnerable to attack by microorganisms such as bacteria and viruses. Amyloid-beta is part of the solution because it allows the astrocytes to be much more effective in utilizing glucose anaerobically, which protects the internally synthesized fats and cholesterol from toxic oxygen exposure, while at the same time providing the energy needed both by the astrocyte for the synthesis process and by neighboring neurons to fuel their signal firings.
Besides the astrocytes, the microglia in the brain are also implicated in Alzheimer’s. Microglia promote neuron growth when all is well, but trigger neuron programmed cell death in the presence of toxic substances secreted by bacteria such as polysaccharides [56]. Microglia will defensively secrete cytokines (communication signals that promote an immune response) when exposed to infective agents, and these in turn will lead to inflammation, another well-known feature associated with Alzheimer’s [1]. The microglia are able to control whether neurons should live or die, and they surely base this decision on factors related to how well the neuron functions and whether it is infected. Once enough neurons have been programmed for cell death, the disease will manifest itself as cognitive decline.
10. Evidence that Infection is Associated with Alzheimer’s
There is substantial evidence that Alzheimer’s is related to an increased likelihood of infective agents appearing in the brain. Some researchers believe that infective agents are the principle cause of Alzheimer’s. There are a number of bacteria that reside in the human digestive system and can co-exist with our own cells without any harm. However, H. pylori, one that is quite common, has been recently shown to be responsible for stomach ulcers. It has been suspected that H. Pylori might be implicated in Alzheimer’s, and, indeed, a recent study showed that Alzheimer’s patients had a significantly higher concentration of an antibody against H. Pylori in both their cerebrospinal fluid and their blood than non-Alzheimer’s controls [26]. H. pylori was detected in 88% of the Alzheimer’s patients but only 47% of the controls. In an effort to treat the Alzheimer’s patients, the researchers administered a potent combination of antibiotics, and assessed the degree of mental decline over the next two years [27]. For 85% of the patients, the infection was successfully routed, and for those patients, cognitive improvement was also detected after two years had elapsed. So this was a nice example of the possibility of treating Alzheimer’s through antibiotics.
C. pneumoniae is a very common bacterium, estimated to infect 40-70% of adults. But there’s a big difference between a bacterium being in the blood stream and making its way into the inner sanctum of the brain. A study of post-mortem samples from various regions of the brains of Alzheimer’s patients and non-Alzheimer’s controls revealed a remarkably different statistic: 17 out of 19 Alzheimer’s brains tested positive for the bacterium, whereas only 1 out of 19 brains from the control group tested positive [5].
Many other infective agents, both viruses and bacteria, have been found to be associated with Alzheimer’s, including herpes simplex virus, picornavirus, Borna disease virus, and spirochete [23]. One proposal was that a particularbacteriophage — a virus that infects the bacterium C. pneumoniae — might be responsible for Alzheimer’s [14]. The authors argued that the phages might make their way into the mitochondria of the host cell and subsequently initiate Alzheimer’s.
11. Ketogenic Diet as Treatment for Alzheimer’s
One of the promising new treatment paradigms for Alzheimer’s is to have the patient switch to an extremely high fat, low carb diet, a so-called “ketogenic” diet. The name comes from the fact that the metabolism of dietary fats produces “ketone bodies” as a by-product, which are a very useful resource for metabolism in the brain. It is becoming increasingly clear that defective glucose metabolism in the brain (so-called “type-3 diabetes”) is an early characteristic of Alzheimer’s. Ketone bodies, whether they enter the astrocyte directly or are produced in the astrocyte itself by breaking down fats, can be delivered to adjacent neurons, as shown in the accompanying figure.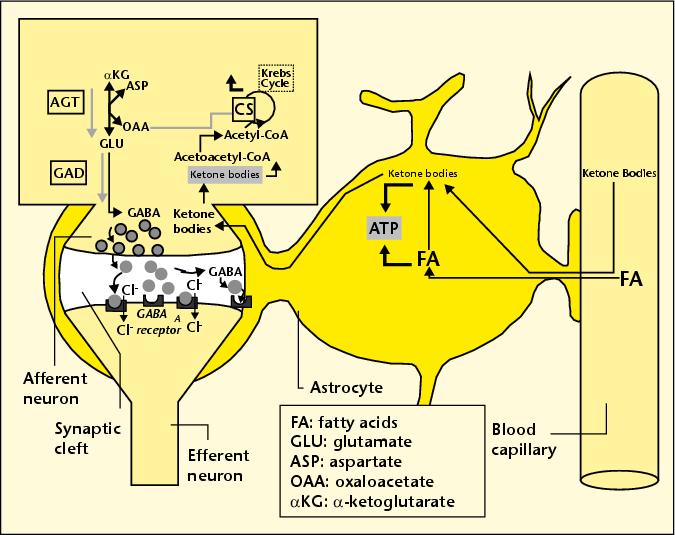 These neurons can utilize the ketone bodies both as an energy source (replacing and therefore relieving glucose) and as a precursor to GABA, a critical neurotransmitter that is widespread in the brain.
These neurons can utilize the ketone bodies both as an energy source (replacing and therefore relieving glucose) and as a precursor to GABA, a critical neurotransmitter that is widespread in the brain.
Evidence that a ketogenic diet might help Alzheimer’s was first found through research conducted on mice who had been bred to be prone to Alzheimer’s disease [21]. Researchers found that the mice’s cognition improved when they were treated with a high-fat low-carb diet, and also that the amount of amyloid-beta in their brain was reduced. The latter effect would be anticipated based on the premise that amyloid-beta promotes full utilization of glucose anaerobically, as I discussed previously. By having ketone bodies as an additional source of fuel, the dependence on glucose is reduced. But another effect that may be more important than this is the availability of high-quality fats to improve the condition of the myelin sheath.
This idea is supported by other experiments done on human Alzheimer’s patients [11] [42]. A placebo-controlled 2004 study [42] of the effect of dietary fat enrichment on Alzheimer’s is especially informative, because it uncovered a significant difference in effectiveness for the fat-enrichment for subjects who did not have the apoE-4 allele as compared with those who did. The experimental test group were given a supplemental drink containing emulsified medium chain triglycerides, found in high concentration in coconut oil. The subjects without the apoE-4 allele showed a significant improvement in score on a standard test for Alzheimer’s, whereas those with the apoE-4 allele did not. This is a strong indicator that the benefit may have to do with an increase in uptake by the astrocyte of these high-quality fats, something that the subjects with the apoE-4 allele are unable to accomplish due to the defective IDL and LDL transport mechanisms.
12. NADH Treatment: the Crucial Role of Antioxidants
One of the very few promising treatments for Alzheimer’s is the coenzyme, NADH (nicotinamide adenine dinucleotide) [12]. In a placebo-controlled study, Alzheimer’s subjects given NADH for six months exhibited significantly better performances on verbal fluency, visual constructional ability and abstract verbal reasoning than the control subjects given a placebo.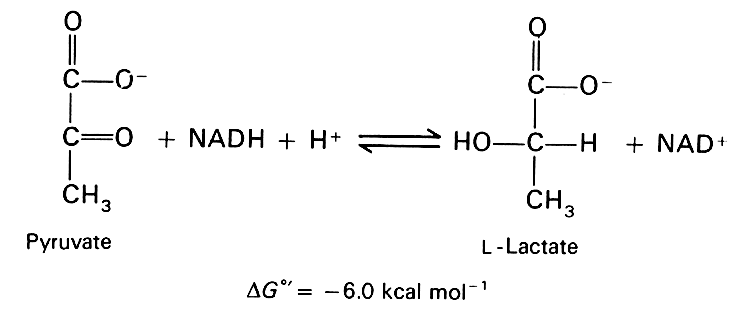
Why would NADH be effective? In the process of converting pyruvate to lactate, lactate dehydrogenase consumes oxygen by oxidizing NADH to NAD+, as illustrated in the accompanying figure. So, if the bioavailability of NADH is increased, it stands to reason that the astrocyte would have an enhanced ability to convert pyruvate to lactate, the critical step in the anaerobic metabolic pathway that is enhanced by amyloid-beta. The process, by absorbing the toxic oxygen, would reduce the damage to the lipids due to oxygen exposure, and would also provide lactate as a source of energy for the neurons.
13. Excessive Oxygen Exposure and Cognitive Decline
It has been observed that some elderly people suffer temporary and sometimes permanent cognitive decline following a lengthy operation. Researchers at the University of South Florida and Vanderbilt University suspected that this might be due to excessive exposure to oxygen [4]. Typically, during an operation, people are often administered high doses of oxygen, even as much as 100% oxygen. The researchers conducted an experiment on young adult mice, which had been engineered to be predisposed towards Alzheimer’s but had not yet suffered cognitive decline. They did however already have amyloid-beta deposits in their brains. The re-engineered mice, as well as a control group that did not have the Alzheimer’s susceptibility gene, were exposed to 100-percent oxygen for a period of three hours, three times over the course of several months, simulating repeated operations. They found that the Alzheimer’s pre-disposed mice suffered significant cognitive decline following the oxygen exposure, by contrast with the control mice.
This is a strong indication that the excessive oxygen exposure during operations is causing oxidative damage in the Alzheimer’s brain. Given the arguments I have presented above, this result makes good sense. The brain, by converting to anaerobic metabolism for generating energy (with help from amyloid-beta) is trying its best to avoid exposing the fatty acids and cholesterol to oxidative damage. But an extremely high concentration of oxygen in the blood makes it very difficult to protect the fats and cholesterol during transport through the blood, and also probably causes an unavoidable increase in oxygen uptake and therefore exposure within the brain itself.
14. Fats are a Healthy Choice!
You would practically have to be as isolated as an Australian Aborigine not to have absorbed the message that dietary fats, particularly saturated fats, are unhealthy. I am extremely confident that this message is false, but it is nearly impossible to turn the opinion tide due to its pervasive presence. Most people don’t question why fats are bad; they assume that researchers must have done their homework, and they trust the result.
To say that the current situation with regard to dietary fats is confusing would be an understatement. We are repeatedly told to keep our total fat intake down to, ideally, 20% of our total calories. This is difficult to achieve, and I believe it is misguided advice. In direct contradiction to this “low-fat” goal, we are encouraged to consume as much as possible of the “good” kinds of fats. Fortunately, the message is finally becoming widely embraced that omega-3 fats are healthy and that trans fats are extremely unhealthy. DHA (docosahexaenoic acid) is an omega-3 fat that is found in large quantities in the healthy brain. In the diet, it is available mainly from cold water fish, but eggs and dairy are also good sources. Trans fats are generated by a high-heat process that hydrolyzes polyunsaturated fats into a more stable configuration, which increases their shelf life but makes them so unnatural they almost can no longer be called a food. Trans fats are extremely damaging both to heart and brain health. A high consumption of trans fats has recently been shown to increase the risk of Alzheimer’s [41]. Trans fats are especially prevalent in highly processed foods — particularly when fats are converted to a powdered form.
We are told to avoid saturated fats, mainly because they have appeared, from empirical evidence, to be more likely to raise LDL levels than unsaturated fats. Yet these fats are less susceptible to oxidation, and this may be why they show up in LDL — because they are of higher quality and therefore should preferentially be delivered to the tissues for functional roles rather than as fuel (i.e., free fatty acids). Coconut oil, a saturated fat, has been shown to benefit Alzheimer’s patients [42]. And high-fat dairy (also highly saturated) has been shown to be beneficial both to fertility among women [10] and, remarkably, to heart disease [37][22].
Despite the widespread belief that fats (particularly saturated fats) are unhealthy, an article that appeared in the American Journal of Clinical Nutrition in 2004 [37] claims that, for a group of post-menopausal women, a high-fat, high-saturated-fat diet affords better protection from coronary artery disease than a low-fat (25% of calories from fats) diet. The subjects in the study were obese women with coronary artery disease. Most of them had high blood pressure, and many had diabetes. They fit the profile for metabolic syndrome that I have previously argued is a direct consequence of a prolonged low-fat high-carb diet. I am gratified to see that my hypothesis that an increase in fat intake would decrease their risk of heart disease has been verified by a carefully controlled study.
Another investigation where fats were shown to afford protection against heart disease has just been completed. It involved a long-term study of a large number of Swedish men [22]. The authors looked at low- vs high-fat dairy, as well as consumption of fruits and vegetables, meats, grains, etc. The only statistically significant result that afforded protection from heart disease was a combination of high-fat dairy and lots of fruits and vegetables. Fruits and vegetables with low-fat dairy afforded no protection.
I suspect one of the critical nutrients the fruits and vegetables provide is antioxidants that help prolong the life of the fats. Other excellent sources of antioxidants include richly colored fruits like berries and tomatoes, coffee, green tea, and dark chocolate, and several spices, most especially cinnamon and turmeric (a major ingredient of curry). These should be consumed in abundance along with fats for optimal results.
Polyunsaturated fats such as corn oil and canola oil are unhealthy for the brain precisely because they are unsaturated. There are two major problems: (1) they have a low melting point, which means that, if they are used for frying they will be converted to trans fats, which are extremely unhealthy, and (2) they are much more susceptible to becoming rancid (oxidized) at room temperature than saturated fats, i.e., they have a shorter shelf life.
Researchers in Germany recently conducted an ingenious experiment designed to determine how the degree of freshness of polyunsaturated fats affects the metabolism of those fats in female lactating rats [43]. They divided female rats into two groups, and the only difference between the test group and the controls was that the test group was given fats that had been left in a relatively warm place for 25 days, which caused considerable oxidative damage, whereas the controls were fed fresh fats instead. The rats’ unusual diet was begun on the day that they gave birth to a litter. The researchers examined the mammary glands and the milk produced by the two groups for apparent differences. They found that the test group’s milk was markedly reduced in the amount of fat it contained, and their mammary glands correspondingly took up less fat from the blood supply. One might surmise that the rats’ metabolic mechanisms were able to detect oxidative damage to the fats, and therefore rejected them, prefering to do without rather than to risk the consequences of feeding their pups oxidized fats. Consequently, the pups of the test group gained significantly less weight than the control group’s pups.
Boxed items like cookies and crackers that contain processed polyunsaturated fats are doctored with antioxidants and even antibiotics to protect them from spoiling. Once they’re consumed, however, they still have to be protected from going rancid. Biochemical laws work the same way whether inside or outside the body. There are plenty of bacteria throughout the body that would be eager to take up house-keeping in rancid fats. The body has devised all kinds of strategies for protecting fats from oxidation (becoming rancid) and from attack by bacteria. But its task is rendered much easier for saturated rather than unsaturated fats, and for fresh rather than stale fats.
If we stop trying to get by on as few fats as possible in the diet, then we don’t have to become so preoccupied with getting the “right” kinds of fats. If the body is supplied with an overabundance of fats, it can pick and choose to find the perfect fat to match each particular need; excess or defective fats can just be used as fuel, where it’s not very important which fat it is, as long as it can be broken down to release energy.
15. Summary and Conclusion
This is an exciting time for Alzheimer’s research, as new and surprising discoveries are coming out at a rapid pace, and evidence is mounting to support the notion that Alzheimer’s is a nutritional deficiency disease. It is an indication of how much progress has been made in recent years to note that 42% of the references in this essay were published in 2008 or 2009. A popular new theory is that Alzheimer’s may grow out of an impaired ability to metabolize glucose in the brain. The term “type-3 diabetes” has been coined to describe this defect, which often appears long before any symptoms of Alzheimer’s [49]. A shift from aerobic towards anaerobic glucose metabolism in the brain seems to be a harbinger of Alzheimer’s later in life, but I argue that the reason for this shift is both to provide a basic ingredient (pyruvate) from which to synthesize fatty acids, while simultaneously protecting them from potentially damaging oxidation. The ApoE-4 allele, which is associated with increased risk to Alzheimer’s, clearly implicates defects in fat and cholesterol transport, and the remarkable 6-fold reduction in the amount of fatty acids present in the cerebrospinal fluid of Alzheimer’s patients [38] speaks loudly the message that fat insufficiency is a key part of the picture. The observation that the myelin is degraded in the frontal lobes of the brains of people possessing the apoE-4 allele further substantiates the theory that the myelin repair mechanism is defective.
Cholesterol obviously plays a vital role in brain function. A whopping 25% of the total cholesterol in the body is found in the brain, and it is present in abundance both in the synapses and in the myelin sheath. The cholesterol in both of these places has been shown to play an absolutely essential role in signal transport and in growth and repair.
Given the strong positive role played by cholesterol, it can only be assumed that statin drugs would increase the risk of developing Alzheimer’s. However, the statin industry has been remarkably successful thus far in hiding this painful fact. They have managed to make much of the observation that high cholesterol much earlier in life is associated with an increased risk to Alzheimer’s thirty years later. Yet they offer not a single study, not even a retrospective study, to substantiate any claim that actively reducing cholesterol through statin therapy would improve the situation for these people. In fact, most damningly, the statin usage evidence that would answer the question was “unavailable” to the researchers who conducted the seminal study.
Beatrice Golomb is an M.D. Ph.D. who heads up the UCSD Statin Study group, a research team who are actively investigating the risk-benefit balance of statin drugs. She is increasingly becoming convinced that statin drugs should not be recommended for the elderly: that in their case the risks clearly outweigh the benefits. She makes a strong case for this position in an on-line article available here [15]. The section on Alzheimer’s is particularly compelling, and it points out the pitfalls in relying on previous studies done by the statin industry, where often those who have memory problems as side-effects of the statin drugs are excluded from the study, so that the results end up inappropriately biased in favor of statins. In summary, she wrote: “It must be emphasized that the randomized trial evidence has, to date, uniformly failed to show cognitive benefits by statins and has supported no effect or frank and significant harm to cognitive function.”
In addition to refusing to take statin therapy, another way in which an individual can improve their odds against Alzheimer’s is to consume plenty of dietary fats. It seems odd to suddenly switch from a “healthy” low-fat diet to an extremely high fat ketogenic diet, once a diagnosis of Alzheimer’s is made. A ketogenic diet consists, ideally, of 88% fat, 10% protein, and 2% carbohydrate [11]. That is to say, it is absurdly high in fat content. It seems much more reasonable to aim for something like 50% fat, 30% protein, and 20% carbohydrate, so as to pro-actively defend against Alzheimer’s.
I highly recommend a recent book written by the pediatric brain surgeon, Larry McCleary, M.D., called The Brain Trust Program [33]. This book gives a wealth of fascinating information about the brain, as well as specific recommendations for ways to improve cognitive function and avert later Alzheimer’s. Most significantly, he recommends a diet that is high in cholesterol and animal fats, including an abundance of fish, seafood, meat, and eggs. He also recommends coconuts, almonds, avocados and cheese, all foods that contain a significant amount of fat, while encouraging the avoidance of “empty carbs.” His knowledge on this subject grew out of his interest in helping his young patients heal more rapidly after brain trauma.
Our nation is currently bracing itself for an onslaught of Alzheimer’s, at a time when baby boomers are approaching retirement, and our health care system is already in a crisis of escalating costs and shrinking funds. We can not afford the high cost of caring for the swelling population of Alzheimer’s patients that our current practices of low-fat diet and ever expanding statin usage are promoting.
Appendix In this appendix, I include the full abstract of two papers that are relevant to the theory presented here. The first is the abstract of reference [19] in [46], which is reference [44] here [see the section on statin drugs above for context]:
Abstract, “Epidemiological and clinical trials evidence about a preventive role for statins in Alzheimer’s disease:”
“This paper reviews epidemiological and clinical trials data about whether statin use reduces the risk of Alzheimer’s disease (AD). The available information has come in three waves. The initial, mostly cross-sectional observational reports suggested that statins might prevent dementia. Next, two large clinical trials with cognitive add-on studies showed no benefit and neither did the third wave, again with observational studies. The latter were mostly longitudinal, and were critical of the first studies for not adequately addressing confounding by indication (i.e. that patients with dementia would be denied statins). Most recently, new data from the Canadian Study of Health and Aging have produced a mixed result. While methodological considerations are clearly important in understanding why the reports are so variable, there might also be merit in differentiating between statins, based on their presumed – and variable – mechanisms of action in dementia prevention, before concluding that the initial reports are entirely artefactual. Still, the first reports appear to have overestimated the extent of protection, so that unless there are important effects achievable with specific statins, a more than a modest role for statins in preventing AD seems unlikely.” The second abstract is taken from reference [28], on the “alternative hypothesis” that amyloid-beta is protective rather than detrimental to Alzheimer’s, i.e., that it is a “protective response to neuronal insult:”
Abstract, “Amyloid-beta in Alzheimer disease: the null versus the alternate hypotheses:”
“For nearly 20 years, the primary focus for researchers studying Alzheimer disease has been centered on amyloid-beta, such that the amyloid cascade hypothesis has become the “null hypothesis.” Indeed, amyloid-beta is, by the current definition of the disease, an obligate player in pathophysiology, is toxic to neurons in vitro, and, perhaps most compelling, is increased by all of the human genetic influences on the disease. Therefore, targeting amyloid-beta is the focus of considerable basic and therapeutic interest. However, an increasingly vocal group of investigators are arriving at an “alternate hypothesis” stating that amyloid-beta, while certainly involved in the disease, is not an initiating event but rather is secondary to other pathogenic events. Furthermore and perhaps most contrary to current thinking, the alternate hypothesis proposes that the role of amyloid-beta is not as a harbinger of death but rather a protective response to neuronal insult. To determine which hypothesis relates best to Alzheimer disease requires a broader view of disease pathogenesis and is discussed herein.”
Contact: seneff@csail.mit.edu
References
[1] H. Akiyama, S. Barger, S. Barnum, B. Bradt, J.Bauer, G.M. Cole, N.R. Cooper, P. Eikelenboom, M. Emmerling, B.L. Fiebich, C.E. Finch, S. Frautschy, W.S. Griffin, H. Hampel, M. Hull, G. Landreth, L. Lue, R. Mrak, I.R. Mackenzie, P.L. McGeer, M.K. O’Banion, J. Pachter, G. Pasinetti, C. Plata-Salaman, J. Rogers, R.Rydel, Y. Shen, W. Streit, R. Strohmeyer, I. Tooyoma, F.L. Van Muiswinkel, R. Veerhuis, D. Walker, S. Webster, B. Wegrzyniak, G. Wenk, and T. Wyss-Coray, “Inflammation and Alzheimer’s disease.” Neurobiol Aging (2000) May-Jun;21(3):383-421,
[2] Alzheimer’s Association, “Alzheimer’s Disease Facts and Figures,” Alzheimer’s and Dementia (2009) Vol. 5, Issue 3.
[3] K.J. Anstey, D.M. Lipnicki and L.F. Low, “Cholesterol as a risk factor for dementia and cognitive decline: a systematic review of prospective studies with meta-analysis.” Am J Geriatr Psychiatry (2008) May, Vol. 16, No. 5, pp. 343-54.
[4] G. Arendash, A. Cox, T. Mori, J. Cracchiolo, K. Hensley, J. Roberts 2nd, “Oxygen treatment triggers cognitive impairment in Alzheimer’s transgenic mice,” Neuroreport. (2009) Jun 18.
[5] B.J. Balin, C.S. Little, C.J. Hammond, D.M. Appelt, J.A. Whittum-Hudson, H.C. Gerard, A.P. Hudson, “Chlamydophila pneumoniae and the etiology of late-onset Alzheimer’s disease.” J. Alz. Dis. (2008) Vol. 13, pp. 371-380.
[6] G. Bartzokis, MD; P.H. Lu, Psy, D.H. Geschwind, MD, N.Edwards, MA, J. Mintz, PhD, and J.L. Cummings, MD, “Apolipoprotein E Genotype and Age-Related Myelin Breakdown in Healthy Individuals: Implications for Cognitive Decline and Dementia,” Arch Gen Psychiatry (2006) Vol. 63, pp. 63-72.
[7] N. Bernoud, L. Fenart, C. Bénistant, J. F. Pageaux, M. P. Dehouck, P. Molière, M. Lagarde, R. Cecchelli,d, and J. Lecerf, “Astrocytes are mainly responsible for the polyunsaturated fatty acid enrichment in blood-brain barrier endothelial cells in vitro” Journal of Lipid Research (1998) Sept., Vol. 39, pp. 1816-1824.
[8] M. S. Brown and J. L. Goldstein, “A Receptor-Mediated Pathway for Cholesterol Homeostasis,” Nobel Lecture, December 9, 1985.
[9] N. Cartier, C. Sevin, A. Benraiss, P. DeDeyn, D. Bonnin, M-T Vanier, M. Philippe, V. Gieselmann and P. Aubourg, “AAV5-Mediated Delivery of Human Aryl Sulfatase A (hARSA) Prevents Sufatide Storage and Neuropathological Phenotype in Metachromatic Leukodystrophy (MLD) Mice,” Molecular Therapy (2005) 11, S166-S167; doi: 10.1016/j.ymthe.2005.06.431
[10] J. Chavarro, W.C. Willett, and P.J. Skerrett, The Fertility Diet, (2008) McGraw Hill.
[11] L.C. Costantini, L.J. Barr, J.L. Vogel and S.T. Henderson, “Hypometabolism as a therapeutic target in Alzheimer’s disease” BMC Neurosci (2008) Vol. 9, Suppl. 2, S16. doi: 10.1186/1471-2202-9-S2-S16.
[12] V. Demarin, S.S. Podobnik, D. Storga-Tomic and G. Kay, “Treatment of Alzheimer’s disease with stabilized oral nicotinamide adenine dinucleotide: A randomized, double-blind study” Drugs Exp Clin Res. (2004) Vol. 30, No. 1, pp. 27-33.
[13] R.B. DeMattos, R.P. Brendza, J.E. Heuser, M.Kierson, J.R. Cirrito, J. Fryer, P.M. Sullivan, A.M. Fagan, X. Han and D.M. Holtzman, “Purification and characterization of astrocyte-secreted apolipoprotein E and J-containing lipoproteins from wild-type and human apoE transgenic mice,” Neurochem Int. (2001) Nov-Dec;39(5-6):415-25. doi:10.1016/S0197-0186(01)00049-3.
[14] M. Dezfulian, M.A. ShokrgozarA, S. Sardari, K. Parivar and G. Javadi, “Can phages cause Alzheimer’s disease?” Med Hypotheses (2008) Nov;71(5):651-6.
[15] B.A. Golomb, M.D., Ph.D., “Statin Adverse Effects: Implications for the Elderly,” Geriatric Times (2004) May/June, Vol. V, Issue 3
[16] W.R. Grant, Ph.D., “Does Vitamin D Reduce the Risk of Dementia?” Journal of Alzheimer’s Disease (2009) May, Vol. 17, No. 1., pp. 151-9.
[17] Dr. Duane Graveline, Lipitor: Thief of Memory, Statin Drugs and the Misguided War on Cholesterol, (2004) http://www.buybooksontheweb.com.
[18] X. Han, “Potential mechanisms contributing to sulfatide depletion at the earliest clinically recognizable stage of Alzheimer’s disease: a tale of shotgun lipidomics,” J Neurochem (2007) November, Vol. 103, Suppl. 1. pp. 171-179. doi: 10.1111/j.1471-4159.2007.04708.x.
[19] X. Han, H. Cheng, J.D. Fryer, A.M. Fagan and D.M. Holtzman, “Novel Role for Apolipoprotein E in the Central Nervous System: Modulation of Sulfatide Content” Journal of Biological Chemistry, March 7, 2003, Vol. 278, pp. 8043-8051, DOI 10.1074/jbc.M212340200.
[20] K. Heininger, “A unifying hypothesis of Alzheimer’s disease. IV. Causation and sequence of events,” Rev Neurosci. (2000) Vol. 11, Spec No, pp.213-328.
[21] S.T. Henderson, “Ketone Bodies as a Therapeutic for Alzheimer’s Disease,” NeuroTherapeutics,, (2008) Jul;5(3):470-80, doi:10.1016/j.nurt.2008.05.004
[22] S. Holmberg, A. Thelin and E.-L. StiernstrNvm, “Food Choices and Coronary Heart Disease: A Population Based Cohort Study of Rural Swedish Men with 12 Years of Follow-up,” Int. J. Environ. Res. Public Health (2009) Vol. 6, pp. 2626-2638;
[23] K. Honjo, R. van Reekum, and N.P. Verhoeff, “Alzheimer’s disease and infection: do infectious agents contribute to progression of Alzheimer’s disease?” Alzheimers Dement. (2009) Jul;5(4):348-60.
[24] S.M. Innis and R.A. Dyer, “Brain astrocyte synthesis of docosahexaenoic acid from n-3 fatty acids is limited at the elongation of docosapentaenoic acid,” (2002) Sept. Journal of Lipid Research, Vol. 43, pp. 1529-1536.
[25] L. Jeng, A.V. Yamshchikov, S.E. Judd, H.M. Blumberg, G.S. Martin, T.R. Ziegler and V. Tangpricha, “Alterations in Vitamin D Status and Anti-microbial Peptide Levels in Patients in the Intensive Care Unit with Sepsis,” Journal of translational Medicine,” (2009) Vol. 7, No. 28.
[26] J. Kountouras, M. Boziki, E. Gavalas, C. Zavos, G. Deretzi, N. Grigoriadis, M. Tsolaki, D. Chatzopoulos, P. Katsinelos, D. Tzilves, A. Zabouri, I. Michailidou, “Increased cerebrospinal fluid Helicobacter pylori antibody in Alzheimer’s disease,” Int J Neurosci. (2009) 119(6):765-77.
[27] J. Kountouras, M. Boziki, E. Gavalas, C. Zavos, N. Grigoriadis, G. Deretzi, D. Tzilves, P. Katsinelos, M. Tsolaki, D. Chatzopoulos, and I. Venizelos, “Eradication of Helicobacter pylori may be beneficial in the management of Alzheimer’s disease,” J Neurol. (2009) May;256(5):758-67. Epub 2009 Feb 25.
[28] H.G. Lee, X. Zhu, R.J. Castellani, A. Nunomura, G. Perry, and M.A. Smith, “Amyloid-beta in Alzheimer disease: the null versus the alternate hypotheses,” J Pharmacol Exp Ther. (2007) June, Vol. 321 No. 3, pp. 823-9. doi:10.3390/ijerph6102626.
[29] J. Marcus, S. Honigbaum, S. Shroff, K. Honke, J. Rosenbluth and J.L. Dupree, “Sulfatide is essential for the maintenance of CNS myelin and axon structure,” Glia (2006), Vol. 53, pp. 372-381.
[30] R.T. Matthews, L. Yang, S. Browne, M. Baik and M.F. Beal, “Coenzyme Q10 administration increases brain mitochondrial concentrations and exerts neuroprotective effects,” Proc Natl Acad Sci U S A. (1998) Jul 21, Vol. 95, No. 15, pp.8892-7.
[31] D. Lutjohann and K. von Bergmann, “24S-hydroxycholesterol: a marker of brain cholesterol metabolism”Pharmacopsychiatry (2003) January 10, Vol. 36 Suppl 2, pp. S102-6, DOI: 10.1055/s-2003-43053.
[32] J. C. McCann and B.N. Ames, “Is there convincing biological or behavioral evidence linking vitamin D deficiency to brain dysfunction?”, (2008) FASEB J. Vol. 22, pp. 982-1001. doi: 10.1096/fj.07-9326rev.
[33] Larry McCleary, M.D., The Brain Trust Program (2007) September, The Penguin Group, New York, New York.
[34] B. McGuinness et al., “Statins for the prevention of dementia,” Cochrane Database of Systematic Reviews,(2009) No. 2.
[35] M.M. Mielke, P.P. Zandi, M. Sjogren, et al. “High total cholesterol levels in late life associated with a reduced risk of dementia,” Neurology (2005) Vol. 64, pp. 1689-1695.
[36] S.A. Moore, “Polyunsaturated Fatty Acid Synthesis and Release by Brain-Derived Cells in Vitro,” Journal of Molecular Neuroscience (2001), Vol. 16, pp. 195ff.
[37] D. Mozaffarian, E.B. Rimm, D.M. Herrington, “Dietary fats, carbohydrate, and progression of coronary atherosclerosis in postmenopausal women,” Am J Clin Nutr (2004) Vol. 80, pp. 1175-84.
[38] M. Mulder, R. Ravid, D.F. Swaab, E.R. de Kloet, E.D. Haasdijk, J. Julk, J.J. van der Boom and L.M. Havekes, “Reduced levels of cholesterol, phospholipids, and fatty acids in cerebrospinal fluid of Alzheimer disease patients are not related to apolipoprotein E4,” Alzheimer Dis Assoc Disord. (1998) Sep, Vol. 12, No. 3, pp. 198-203.
[39] I.L. Notkola, R. Sulkava, J. Pekkanen, T. Erkinjuntti, C. Ehnholm, P. Kivinen, J. Tuomilehto, and A. Nissinen, “Serum total cholesterol, apolipoprotein E epsilon 4 allele, and Alzheimer’s disease,” Neuroepidemiology (1998) Vol. 17, No. 1, pp. 14-20.
[40] F.W. Pfrieger, “Outsourcing in the brain: Do neurons depend on cholesterol delivery by astrocytes?”, BioEssays(2003) Vol. 25 Issue 1, pp.72-78.
[41] A. Phivilay, C. Julien, C. Tremblay, L. Berthiaume, P. Julien, Y. Giguère and F. Calon, “High dietary consumption of trans fatty acids decreases brain docosahexaenoic acid but does not alter amyloid-beta and tau pathologies in the 3xTg-AD model of Alzheimer’s disease.” Neuroscience (2009) Mar 3, Vol. 159, No. 1, pp. 296-307. Epub 2008 Dec 14.
[42] M.A. Reger, S. T. Henderson, C. Hale, B. Cholerton, L.D. Baker, G.S. Watson, K. Hyde, D. Chapman and S. Craft, “Effects of Beta-hydroxybutyrate on cognition in memory-impaired adults,” Neurobiology of Aging (2004) Vol. 25, No. 3, March, pp. 311-314,
[43] R. Ringseis, C. Dathe, A. Muschick, C. Brandsch and K. Eder, “Nutrient Physiology, Metabolism, and Nutrient-Nutrient Interactions Oxidized Fat Reduces Milk Triacylglycerol Concentrations by Inhibiting Gene Expression of Lipoprotein Lipase and Fatty Acid Transporters in the Mammary Gland of Rats,” American Society for Nutrition J. Nutr. (2007) Sept., Vol. 137, pp. 2056-2061.
[44] K. Rockwood, “Epidemiological and clinical trials evidence about a preventive role for statins in Alzheimer’s disease.” Acta Neurol Scand Suppl. (2006) Vol. 185, pp. 71-7.
[45] G. Saher, B. Brugger, C. Lappe-Siefke, W. Mobius, R. Tozawa, M.C. Wehr, F. Wieland, S. Ishibashi, and K.A. Nave, “High cholesterol level is essential for myelin membrane growth.” Nat Neurosci (2005) Apr, Vol. 8, No. 4, pp. 468-75. Epub 2005 Mar 27.
[46] A. Solomon, M. Kivipelto, B. Wolozin, J. Zhou, and R.A. Whitmer, “Midlife Serum Cholesterol and Increased Risk of Alzheimer’s and Vascular Dementia Three Decades Later,” Dementia and Geriatric Cognitive Disorders (2009) Vol. 28, pp. 75-80, DOI: 10:1159/000231980.
[47] M. Simons, MD, P. Keller, PhD, J. Dichgans, MD and J.B. Schulz, MD, “Cholesterol and Alzheimer’s disease: Is there a link?” Neurology (2001) Vol. 57, pp. 1089-1093.
[48] L.L. Smith, “Another cholesterol hypothesis: cholesterol as antioxidant,” Free Radic Biol Med. (1991) Vol. 11, No. 1, pp. 47-61.
[49] E. Steen, B.M. Terry, E.J. Rivera, J.L. Cannon, T.R. Neely, R. Tavares, X.J. Xu, J.R. Wands, and S.M. de la Monte “Impaired insulin and insulin-like growth factor expression and signaling mechanisms in Alzheimer’s disease – is this type 3 diabetes?” Journal of Alzheiner’s Disease (2005) Vol. 7, Number 1, pp. 63-80.
[50] J. Tong, P.P. Borbat, J.H. Freed and Y-K Shin, “A scissors mechanism for stimulation of SNARE-mediated lipid mixing by cholesterol,” PNAS (2009) March 31 Vol. 106, No. 13, pp. 5141-5146.
[51] M-C Vohl, T. A.-M. Neville, R. Kumarathasan, S. Braschi, and D.L. Sparks, “A Novel Lecithin-Cholesterol Acyltransferase Antioxidant Activity Prevents the Formation of Oxidized Lipids during Lipoprotein Oxidation,”Biochemistry (1999) Vol. 38 No. 19, pp. 5976-5981. DOI: 10.1021/bi982258w.
[52] M. Waldman, MD,, 9th International Conference on Alzheimer’s and Parkinson’s Diseases (2009) Abstract 90, Presented March 12-13.
[53] R. West, M.A., M. Schnaider Beeri, Ph.D., J. Schmeidler, Ph.D., C. M. Hannigan, B.S., G. Angelo, M.S., H.T. Grossman, M.D., C. Rosendorff, M.D., Ph.D., and J.M. Silverman, Ph.D., “Better memory functioning associated with higher total and LDL cholesterol levels in very elderly subjects without the APOE4 allele,” Am J Geriatr Psychiatry(2008) September; Vol. 16, No. 9, pp. 781-785. doi: 10.1097/JGP.0b013e3181812790.
[54] A.W.E. Weverling-Rijnsburger, G.J. Blauw, A.M. Lagaay, D.L. Knook, A.E. Meinders, and R.G.J. Westendorp, “Total cholesterol and risk of mortality in the oldest old,” The Lancet, (1997) Vol. 350, No. 9085, pp. 1119-1123,
[55] R.F. Wilson, J.F. Barletta and J.G. Tyburski, “Hypocholesterolemia in Sepsis and Critically Ill or Injured Patients”Critical Care (2003), Vol. 7, pp. 413-414.
[56] S.-C. Zhang and S. Fedoroff, “Neuron-microglia Interactions in Vitro,” Acta Neuropathol (1996) Vol. 91, pp. 385-395.
September 20, 2021 Posted by aletho | Book Review, Science and Pseudo-Science, Timeless or most popular | alzheimer's, Cholesterol, Statins, Vitamin D | Leave a comment
T-Cells Really Are The Superstars In Fighting COVID-19
British Medical Journal | Septmber 17, 2020
Thank you to Dr Doshi for raising the profile of T-cells. Incidentally, German researchers found that a staggering 81 percent of individuals had pre-existing T-cells that cross-react with SARS-CoV-2 epitopes [1].
This fits with modelling in May by Imperial College’s Professor Friston, a world authority in mathematical modelling of complex dynamic biological systems, indicating that around 80% and 50% of the German and UK populations, respectively, are resistant to COVID-19: https://unherd.com/2020/06/karl-friston-up-to-80-not-even-susceptible-to…
Antibodies can only latch onto and help destroy pathogens outside cells and may also occasionally, paradoxically, enhance a pathogen’s ability to infect cell instead by antibody dependent ”enhancement” or ADE. It is only the T-cell that can cleverly sense and destroy pathogens inside infected cells using “sensors” which detect foreign protein fragments.
In the late 60’s the Lancet described a case of a child with agammaglobulinemia, a condition in which absence of B cells prevent them from producing antibodies, who overcame a measles infection quite normally and did not become re-infected thereafter. We now know that, although this condition can compromise immunity, in that particular case the rest of the immune functions, including T-cells, must have been perfectly up to the job of clearing infection and establishing immune memory without help from antibodies.
The importance of T-cells in fighting SARS-CoV-1 and establishing immune memory has also been well documented and discussed in a number of pre-COVID papers from 2017 and earlier [2].
Then, early in April, it was reported that two patients with agammaglobulinemia overcame COVID-19 infections without requiring ventilation [3], prompting the Italian authors to write: “This observation suggests that T‐cell response is probably important for immune protection against the virus, while B‐cell response might be unessential”.
All this should have shifted the focus of efforts towards T-cells at an early stage – the real question is why mainstream media and others continued to focus efforts and narrative on antibodies. Is it because vaccines are good at provoking antibody responses but not so great at generating T-cells? Some of the vaccines presently under trial do elicit some T-cells but it seems that neither the quantity nor variety are hugely impressive.
Does this matter? Apparently so: Research establishments including Yale found that in mild or asymptomatic cases, many T-cells are produced. These were highly varied, responding not just to parts of the Spike, S protein or Receptor Binding Domain but to many other parts of the virus [1, 4-6]. Notably, in these mild cases there were few or no detectable antibodies.
Conversely, the severely ill produced few T-cells with less variety but had plenty of antibodies. What is also of interest is that men produced fewer T-cells than women, and unlike women, their T-cell response reduced with age [7].
So why are some people unable to mount a good protective T-cell response? The key to this question might be a 10-year-old Danish study led by Carsten Geisler, head of the Department of International Health, Immunology and Microbiology at the University of Copenhagen [8].
Geisler noted that “When a T cell is exposed to a foreign pathogen, it extends a signalling device or ‘antenna’ known as a vitamin D receptor, with which it searches for vitamin D,”, and if there is an inadequate vitamin D level, “they won’t even begin to mobilize.” In other words, adequate vitamin D is critically important for the activation of T-cells from their inactive naïve state.
The question of whether T-cells might also need a continuing supply of vitamin D to prevent the T-cell exhaustion and apoptosis observed in some serious COVID-19 cases [9] deserves further research.
High levels of vitamin D are also critical for first line immune defences including physical mucosal defences, human antiviral production, modulating cytokines, reducing blood clotting and a whole host of other important immune system functions [10]. The obese, diabetics and people of BAME origin are far more deficient in vitamin D and men have lower levels than women [10].
Another intriguing clue is that Japan has the highest proportion of elderly on the planet but despite lack of lockdowns, little mask wearing and high population densities in cities, it escaped with few COVID deaths. Could this, at least in part, be because of extraordinarily high vitamin D levels of over 30 ng/ml in 95% of the active elderly [11]? By comparison, UK average levels are below 20ng/ml [10].
Vitamin D is made in the skin from the action of UV sunlight, food usually being a poor source, but the Japanese diet includes unusually high levels. Sunny countries near the equator (e.g. Nigeria, Singapore, Sri Lanka) also have very low COVID related deaths.
The results of the first vitamin D intervention double blind RCT for COVID was published on 29 August by researchers in Córdoba, Spain. This very well conducted study produced spectacular outcomes for the vitamin D group (n=50), virtually eliminating the need for ICU (reducing it by 96%) and eliminating deaths (8% in the n=26 control group). Although this was a small trial, the ICU results are so dramatic that they are statistically highly significant [12].
Substantially more vitamin D is required for optimal immune function than for bone health. It seems Dr Fauci is not ignorant of this, having apparently confirmed on TV and by email that he takes 6,000 IU daily! (see Dr John Campbell on YouTube Vitamin D and pandemic science, 16 September 2020). Meanwhile the US’s health body continues to recommend only 600-800 IU and the UK’s, only 400 IU.
It is high time for joined up solid scientific rationale to overthrow mainstream narratives based on an alternative “science” controlled by industry interests/politics. Beda M Stadler, the former Director of the Institute for Immunology at the University of Bern, a biologist and Professor Emeritus, certainly appears to think so (see Ivor Cummins Ep91 Emeritus Professor of Immunology… Reveals Crucial Viral Immunity Reality on YouTube, 28 July 2020).
In the same way that prior infections protect us against future infections by means of cross-reacting T-cells, overcoming COVID-19 naturally offers potential for greater protection against future coronaviruses. Vaccines have their place but so do our amazingly complex, sophisticated, highly effective immune systems which have evolved over millennia to protect us from a world teeming with trillions of pathogens.
References
- Annika Nelde, Tatjana Bilich, Jonas S. Heitmann et al. SARS-CoV-2 T-cell epitopes define heterologous and COVID-19-induced T-cell recognition, 16 June 2020, Research Square https://www.researchsquare.com/article/rs-35331/v1%20
- William J.Liuabc et al. T-cell immunity of SARS-CoV: Implications for vaccine development against MERS-CoV.Antiviral Research. Volume 137, January 2017, Pages 82-92 https://doi.org/10.1016/j.antiviral.2016.11.006
- Soresina, A, Moratto, D, Chiarini, M, et al. Two X‐linked agammaglobulinemia patients develop pneumonia as COVID‐19 manifestation but recover. Pediatr Allergy Immunol. 2020; 31: 565– 569. https://doi.org/10.1111/pai.13263
- Avraham Unterman, et al. Single-Cell Omics Reveals Dyssynchrony of the Innate and Adaptive Immune System in Progressive COVID-19. medRxiv 2020.07.16.20153437; doi: https://doi.org/10.1101/2020.07.16.20153437
- Leticia Kuri-Cervantes, et al. Immunologic perturbations in severe COVID-19/SARS-CoV-2 infection. bioRxiv 2020.05.18.101717; doi: https://doi.org/10.1101/2020.05.18.101717
- Floriane Gallais, Aurelie Velay, Marie-Josee Wendling, Charlotte Nazon, Marialuisa Partisani, Jean Sibilia, Sophie Candon, Samira Fafi-Kremer. Intrafamilial Exposure to SARS-CoV-2 Induces Cellular Immune Response without Seroconversion. medRxiv 2020.06.21.20132449; doi: https://doi.org/10.1101/2020.06.21.20132449
- Takahashi T, Wong P, Ellingson M, et al. Sex differences in immune responses to SARS-CoV-2 that underlie disease outcomes. Preprint. medRxiv. 2020;2020.06.06.20123414. Published 2020 Jun 9. doi:10.1101/2020.06.06.20123414
- Von Essen MR, Kongsbak M, Schjerling P, Olgaard K, Odum N, Geisler C. Vitamin D controls T cell antigen receptor signaling and activation of human T cells. Nat Immunol. 2010;11(4):344-349. doi:10.1038/ni.1851
- Diao B, Wang C, Tan Y, et al. Reduction and Functional Exhaustion of T Cells in Patients With Coronavirus Disease 2019 (COVID-19). Front Immunol. 2020;11:827. Published 2020 May 1. doi:10.3389/fimmu.2020.00827
- King, E.. The Role of Vitamin D deficiency in COVID-19 related deaths in BAME, Obese and Other High-risk Categories. 2020, June 17. https://doi.org/10.31232/osf.io/73whx
- Nakamura K. Vitamin D insufficiency in Japanese populations: from the viewpoint of the prevention of osteoporosis. J Bone Miner Metab. 2006;24(1):1-6. doi:10.1007/s00774-005-0637-0
- Marta Entrenas Castillo et al. Effect of calcifediol treatment and best available therapy versus best available therapy on intensive care unit admission and mortality among patients hospitalized for COVID-19: A pilot randomized clinical study. The Journal of Steroid Biochemistry and Molecular Biology. Volume 203, October 2020, 105751. https://doi.org/10.1016/j.jsbmb.2020.105751
August 31, 2021 Posted by aletho | Science and Pseudo-Science, Timeless or most popular | Covid-19, Vitamin D | Leave a comment
Children who drink whole milk are leaner and have higher vitamin D levels, new research suggests
ST. MICHAEL’S HOSPITAL | November 16, 2016
TORONTO – Children who drink whole milk are leaner and have higher vitamin D levels than those who drink low-fat or skim milk, new research suggests.
Children who drank whole (3.25 per cent fat content) milk had a Body Mass Index score that was 0.72 units lower than those who drank 1 or 2 per cent milk in the study published today in the American Journal of Clinical Nutrition.
That’s comparable to the difference between having a healthy weight and being overweight, said lead author Dr. Jonathon Maguire, a pediatrician at St. Michael’s Hospital.
The study did not assess why consuming higher fat content milk was associated with lower BMI scores. But Dr. Maguire hypothesized that children who drank whole milk felt fuller than those who drank the same amount of low-fat or skim milk. If children don’t feel full from drinking milk, they are more likely to eat other foods that are less healthy or higher in calories, said Dr. Maguire. Therefore children who drink lower fat milk may actually consume more calories overall than those who drink whole milk.
The study also found that children who drank one cup of whole milk each day had comparable vitamin D levels to those who drank nearly 3 cups of one per cent milk. This could be because vitamin D is fat soluble, meaning it dissolves in fat rather than water. Milk with higher fat content therefore contains more vitamin D. There may also be an inverse relationship in children between body fat and vitamin D stores, according to the study; as children’s body fat increases, their vitamin D stores decrease.
“Children who drink lower fat milk don’t have less body fat, and they also don’t benefit from the higher vitamin D levels in whole milk,” said Dr. Maguire. “It’s a double negative with low fat milk.”
The study’s findings differ from Health Canada, National Institutes of Health and American Academy of Pediatrics guidelines recommending two servings of low fat (one per cent or two per cent) milk for children over the age of two to reduce the risk of childhood obesity.
Dr. Maguire said the findings indicated a need to closely examine existing nutritional guidelines around milk fat consumption to make sure they are having the desired effect. Childhood obesity has tripled in the past 30 years while consumption of whole milk has halved over the same period.
“What kind of milk our children should be consuming is something we need to seek the right answer for,” said Dr. Maguire.
For this study, researchers studied 2,745 children ages two to six years attending well-child visits. They surveyed parents, measured height and weight to calculate BMI and took blood samples to assess vitamin D levels. All were enrolled in the Applied Research Group for Kids (TARGet Kids!), collaboration between children’s doctors and researchers from St. Michael’s Hospital and The Hospital for Sick Children. The program follows children from birth with the aim of preventing common problems in the early years and understanding their impact on health and disease later in life.
Of those studied, 49 per cent drank whole milk, 35 per cent drank two per cent milk, 12 per cent drank one per cent milk and four per cent drank skim milk. Less than one per cent of children drank some combination of the four types of milk.
November 16, 2016 Posted by aletho | Science and Pseudo-Science, Timeless or most popular | Vitamin D | Leave a comment
Featured Video
Larry Johnson: U.S. Desperation Grows as Iran Is Winning
or go to
Aletho News Archives – Video-Images
From the Archives
A low-fat, high-carb diet has been the largest public health experiment in history. It’s past time for a rethink.
By Malcolm Kendrick | RT | November 25, 2020
New research suggests that four billion people globally will be overweight in 2050. This trend can be traced back to the ‘low-fat, high-carb’ guidelines first issued in the 70s, and should prompt a major U-turn on dietary advice.
A recent report from the Potsdam Institute predicts that by 2050 there will be four billion overweight people in the world, with one-and-a-half billion of them obese. This is not entirely surprising. The world has been getting fatter for years, and things do not seem to be slowing down.
Why is this happening? … continue
Blog Roll
-
Join 2,459 other subscribers
Visits Since December 2009
- 7,487,727 hits
Looking for something?
Archives
Calendar
May 2026 M T W T F S S 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 Categories
Aletho News Civil Liberties Corruption Deception Economics Environmentalism Ethnic Cleansing, Racism, Zionism Fake News False Flag Terrorism Full Spectrum Dominance Illegal Occupation Mainstream Media, Warmongering Malthusian Ideology, Phony Scarcity Militarism Progressive Hypocrite Russophobia Science and Pseudo-Science Solidarity and Activism Subjugation - Torture Supremacism, Social Darwinism Timeless or most popular Video War Crimes Wars for IsraelTags
9/11 Afghanistan Africa al-Qaeda Australia BBC Benjamin Netanyahu Brazil Canada CDC Central Intelligence Agency China CIA CNN Covid-19 COVID-19 Vaccine Donald Trump Egypt European Union Facebook FBI FDA France Gaza Germany Google Hamas Hebron Hezbollah Hillary Clinton Human rights Hungary India Iran Iraq ISIS Israel Israeli settlement Japan Jerusalem Joe Biden Korea Latin America Lebanon Libya Middle East National Security Agency NATO New York Times North Korea NSA Obama Pakistan Palestine Poland Qatar Russia Sanctions against Iran Saudi Arabia Syria The Guardian Turkey Twitter UAE UK Ukraine United Nations United States USA Venezuela Washington Post West Bank WHO Yemen Zionism
 Aletho News
Aletho News- Pirates of Mediterranean: Israel does as it pleases in the Sea of Three Continents
- Minab children massacre not ‘unfortunate situation’ but ‘heinous war crime’: Tehran
- OPCW Forced To Pay Damages To Whistleblower Who Found Evidence Of False Flag In Syria
- Iran can thrive under blockade, the US and its allies cannot
- Iran slams US leadership, debunking fabrications, false war costs
- Here’s why Iran is sovereign and Germany is not
- Israel pours $730m into global propaganda machine as reputation collapses
- Leaked audios reveal pro-Israel groups ‘paid’ for US pardon of convicted drug trafficker Juan Orlando Hernandez
- Congress Extends Section 702 Spy Program 45 Days
- Zionists Are Gunning for Your Freedom of Speech
 If Americans Knew
If Americans Knew- Israel conducts farthest-ever strike in long history of attacks on Gaza humanitarian aid flotillas
- In Gaza, Israel commits 10+ ceasefire violations a day – Daily Update
- US ships 6,500 tons of munitions, equipment to Israel in 24 hours
- A New Library in Gaza Rises From the Ashes of Destruction
- Israel’s top Jewish religious body ‘refuses to condemn’ smashing of Jesus statue
- Nun assaulted in Jerusalem amid ‘pattern’ of anti-Christian attacks by Israelis
- Former Tik Tok official describes massive pressure from Israel lobby
- Amid ceasefire violations and genocide, Israel commits piracy – Daily Update
- Five Laws and Standards That Require the US Cut Off Weapons to Israel
- Israel’s diabolical killing machine and how it targets journalists.
 No Tricks Zone
No Tricks Zone- Oversupply Of Volatile Solar Energy Leads To Record NEGATIVE Prices!
- New Study: Extreme Heat Records, Heatwaves, Extreme Cold Records Declining Across US Since 1899
- It’s The Cold, Stupid! Cold 20 Times More Lethal Than Heat, Multiple Studies Show
- European Institute For Climate And Energy: “Climate Debate is Seldom About Science”
- New Study: The Climate May Be 5 Times More Sensitive To Solar Forcing Than Commonly Assumed
- EV Industry Reached $70 Billion In Losses In 2024 Due To Delusional Green Ideologies
- Reality Check: Maldives Have Actually Grown In Size Or Remained Stable Over Recent Decades
- Abrupt Climate Change Also Occurred NATURALLY In The Past …25 Times During Last Ice Age
- Cave Discovery Reveals Today’s Desert Climates Were Recently Far Warmer, Wetter, Teeming With Life
- German Expert: Heat Dome Led To Record Temps In Western USA…Warmer In 1934, 1936
Contact:
atheonews (at) gmail.com
Disclaimer
This site is provided as a research and reference tool. Although we make every reasonable effort to ensure that the information and data provided at this site are useful, accurate, and current, we cannot guarantee that the information and data provided here will be error-free. By using this site, you assume all responsibility for and risk arising from your use of and reliance upon the contents of this site.
This site and the information available through it do not, and are not intended to constitute legal advice. Should you require legal advice, you should consult your own attorney.
Nothing within this site or linked to by this site constitutes investment advice or medical advice.
Materials accessible from or added to this site by third parties, such as comments posted, are strictly the responsibility of the third party who added such materials or made them accessible and we neither endorse nor undertake to control, monitor, edit or assume responsibility for any such third-party material.
The posting of stories, commentaries, reports, documents and links (embedded or otherwise) on this site does not in any way, shape or form, implied or otherwise, necessarily express or suggest endorsement or support of any of such posted material or parts therein.
The word “alleged” is deemed to occur before the word “fraud.” Since the rule of law still applies. To peasants, at least.
Fair Use
This site contains copyrighted material the use of which has not always been specifically authorized by the copyright owner. We are making such material available in our efforts to advance understanding of environmental, political, human rights, economic, democracy, scientific, and social justice issues, etc. We believe this constitutes a ‘fair use’ of any such copyrighted material as provided for in section 107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section 107, the material on this site is distributed without profit to those who have expressed a prior interest in receiving the included information for research and educational purposes. For more info go to: http://www.law.cornell.edu/uscode/17/107.shtml. If you wish to use copyrighted material from this site for purposes of your own that go beyond ‘fair use’, you must obtain permission from the copyright owner.
DMCA Contact
This is information for anyone that wishes to challenge our “fair use” of copyrighted material.
If you are a legal copyright holder or a designated agent for such and you believe that content residing on or accessible through our website infringes a copyright and falls outside the boundaries of “Fair Use”, please send a notice of infringement by contacting atheonews@gmail.com.
We will respond and take necessary action immediately.
If notice is given of an alleged copyright violation we will act expeditiously to remove or disable access to the material(s) in question.
All 3rd party material posted on this website is copyright the respective owners / authors. Aletho News makes no claim of copyright on such material.
